The five deadliest cancers for women: Lung cancer
Lung cancer is the most deadly cancer’and 90 percent of cases can be attributed to smoking
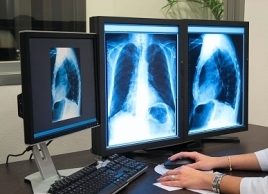
Source: Best Health Magazine, October 2008
‘Women continue to smoke, so the incidence of lung cancer among women is on the rise. Men have cut back,’ says Dr. Yee Ung, a radiation oncologist at the Sunnybrook Odette Cancer Centre in Toronto.
Gail Pfaff of Thunder Bay, Ont., had been smoking since back when she was a teenager. In August 2004, at age 52, she was diagnosed with small-cell lung cancer‘a very aggressive form of the disease. ‘I really didn’t think I would see age 53,’ she says.
Pfaff’s tumour was in the middle of her chest, and she was told that surgery would simply be too risky. So instead, her doctors gave her radiation and powerful chemotherapy. Four years after her cancer diagnosis, she has recovered and has returned to her job as an educational assistant. She is now cancer-free.
A major issue in lung cancer is deciding which treatments should be given to patients like Pfaff. At the recent American Society of Clinical Oncology meeting in Chicago, Dr. Donna Maziak and her colleagues from the Ontario Clinical Oncology Group announced the results of a large study that compared the use of PET scans to biopsies of the lymph nodes in the chest to determine whether patients are good candidates for surgery.
They concluded that PET scanning better identifies the lung cancers that are too advanced for surgery, providing doctors with the information they need to decide on the most appropriate treatment for each individual patient.
Another focus of lung cancer research is earlier detection of the disease. When diagnosed at Stage 1, the five-year survival rate is 60 to 70 percent; by Stage 3, it’s about 15 percent. German researchers at the University Clinic of Cologne recently announced that they have developed a promising new blood test to detect lung cancer. However, it will require further study before becoming widely available.
Dr. Ming Tsao, a pathologist and senior scientist at the Princess Margaret Hospital and the Ontario Cancer Institute in Toronto, is another leading Canadian researcher. He and his colleagues have recently discovered a way to classify people who have non-small-cell lung cancer’this particular type accounts for 80 percent of cases’into those who are and those who are not likely to benefit from chemotherapy after surgery, by doing a genetic analysis of their tumour.
‘This is an exciting discovery,’ says Tsao, explaining that the method would be more accurate than the series of stages that are currently used to determine which patients might benefit from chemotherapy. Those who would not could be spared the toxic therapy.
Read more about the new discoveries, treatments, current studies and diagnostic tools for other deadly cancers:
Breast Cancer
Pancreatic Cancer
Colorectal Cancer
Ovarian Cancer
Found this article informative? Subscribe to our magazine today and receive more Best Health exclusives delivered to your door!




