
Should I avoid certain foods while taking meds?
There are some food-drug interactions that can occur when you eat food while taking certain meds. For example, milk can interfere with some antibiotics and you may want to avoid bananas and other high potassium foods if you’re taking meds for high blood pressure or diuretics for excess fluid retention. “Eating foods high in potassium can increase the risk of irregular heartbeat or palpitations because they increase the amount of potassium in your body,” says Jeremy Allen, MD, the medical director for American Family Care‘s Birmingham, Alabama region. Other well-known interactions include grapefruit juice with statins and overloading on vitamin K or cranberries with blood thinners, such as Warfarin.
For more information on food interactions, check out this booklet published by the U.S. Food and Drug Administration (FDA).
Can I still have a glass of wine when I’m taking meds?
Drinking alcohol when you don’t take meds changes things in your body—there’s the buzz factor, drowsiness, possible hangovers, changes in your blood sugar, and more. Drinking alcohol will increase the instance of side effects with certain meds. For example, you could become very drowsy if you sip wine and take allergy meds. Tyramine, a component found in many alcoholic beverages as a result of the fermentation process, can cause a sudden, unsafe increase in your blood pressure if you’re taking meds such as antibiotics, antipsychotics, antifungals, and monoamine oxidase inhibitors (MAOIs). “In cases of some antibiotics and antifungals, alcohol intake can also cause nausea, stomach cramps, vomiting, flushing, and headaches,” says Dr. Allen.

I threw up. Should I take another dose or wait?
When did you take the meds? “If you vomit within 15 minutes of taking your medication, you should definitely take another dose, because it likely hasn’t been digested,” recommends Dr. Allen. If it has been more than an hour or two, your meds have probably already passed your stomach, so you can wait till your next dose is due. However, you should call your doctor if you’re not sure, because the risk of missing a dose may trump the risk of having additional medicine in your bloodstream. (If your meds are giving you tummy trouble, you may want to try these home remedies to help soothe your stomach.)

How long will it take for me to feel the effects?
When you’re sick and tired of being sick and tired, you want relief fast but feeling better may take longer, depending on your condition and the medication. Some meds travel straight from your digestive systems to your bloodstream while others have to get through the liver first. “Medication will typically reach your bloodstream no later than eight hours after you’ve ingested it, but in some cases, it will reach peak levels in your blood after only 30 minutes,” says Dr. Allen. If you’re taking a time-release med, these are designed to dissolve slowly and give your body stable levels of the meds throughout the day. “You should begin to feel effects from the medication within the first six to eight hours, but it might take sustained ingestion to make a significant difference in your condition.”
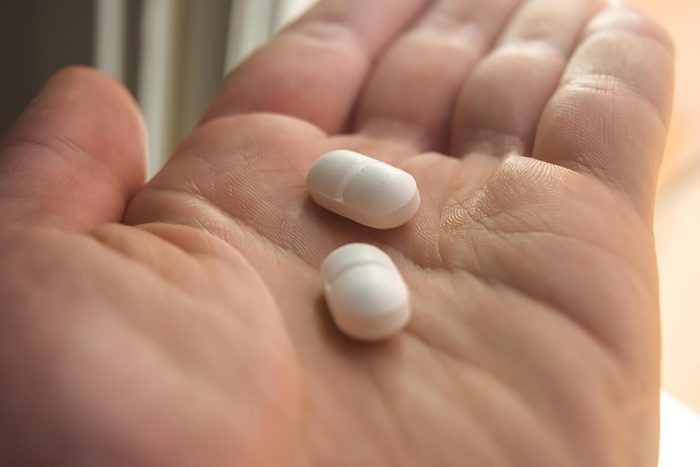
Can I crush my pills to make them easier to swallow?
It’s not just kids who hate to swallow pills, some adults find the prospect of swallowing a pill overwhelming. In most cases, it’s OK to crush the pill and mix it with applesauce or pudding, but Dr. Allen says that’s a no-no with meds that are slow-dissolving or have time-release coatings that could lead to an overdose of the medication or irritate your stomach lining.

Do I have to take the full course of meds?
According to Marc I. Leavey, MD, a primary care specialist at Lutherville Personal Physicians, a Mercy Medical Center Community Physician Site, it depends on the type of condition you have. If you’re taking meds to relieve pain and the pain goes away, you can probably stop taking the pills, unless it is the only thing controlling the pain. If you’re taking antibiotics for an infection, however, stick with the course. “There may be residual bacteria holding on despite the onslaught of antibiotics, ready to multiply should the medication be stopped too soon,” cautions Dr. Leavey.
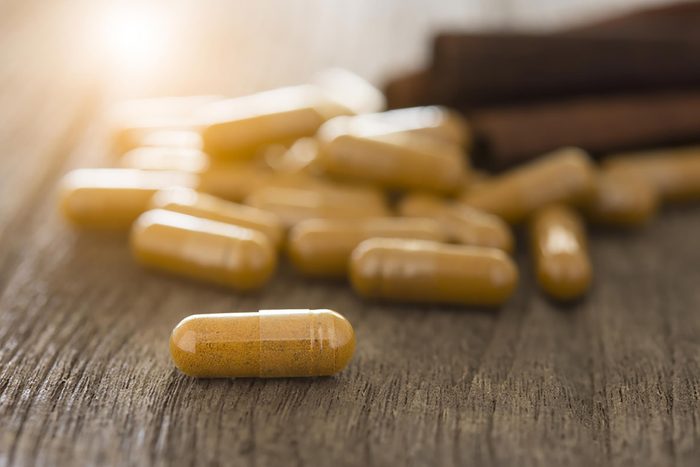
Will my supplements and herbs conflict with my meds?
Healing herbs and supplements have been used for hundreds of years to prevent and combat illness, but these same all-natural products can be dangerous when mixed with prescription meds. “Some vitamins and herbs can interact with certain medications, which may change how the medication works and/or can cause dangerous side effects,” says Jamie Chan, Pharm.D., executive director, pharmacy quality & medication safety at Kaiser Permanente. The list is so long for interactions that it is essential you tell your doctor everything you are taking, even if it is “all-natural.” Your doctor and pharmacist will have an interaction checker to verify if your supplements, herbs, or vitamins will conflict with your medications. (Keep in mind, these five key supplements can benefit every woman.)

Should I take probiotics while I’m taking antibiotics?
If you’ve ever had troublesome side effects to taking antibiotics like bloating, constipation, diarrhea, or a yeast infection, you know how miserable it can be to be sick and have these symptoms on top of everything else. Kent Holtorf, MD, medical director at Holtorf Medical Group, suggests his patients take probiotics. “When taking antibiotics, higher doses of probiotics are needed because the makeup of the bacteria in your gut is essentially a competition. As the antibiotics kill off some of the good bacteria, more bad bacteria can take hold,” says Dr. Holtorf. “It is best to take the probiotic as far away from the antibiotic as possible to lessen the amount of good bacteria in the probiotic being killed, but killing some is unavoidable.” To power up the good bacteria fight, Dr. Holtorf recommends at least 200 to 400 billion colony forming units (CFU’s) during and for several weeks after taking antibiotics. “It is very safe and almost never associated with any problems,” he says. (Psst: Probiotics can also be found in these foods.)

Does take “twice a day” mean every 12 hrs or morning and evening?
According to Dr. Leavey, the common practice, even in hospitals is breakfast and dinner time. If your label directs you to take the meds three times a day that equates to morning, afternoon, and evening. “It likely never hurts to be more precise, but using the less accurate twice daily times instead of every 12 hours may cause some drugs to be incorrectly dosed,” says Dr. Leavey. Letting meds fully leave your bloodstream could alter your treatment. Of course, this is a general rule of thumb and you should ask your doctor or pharmacist if you are concerned.
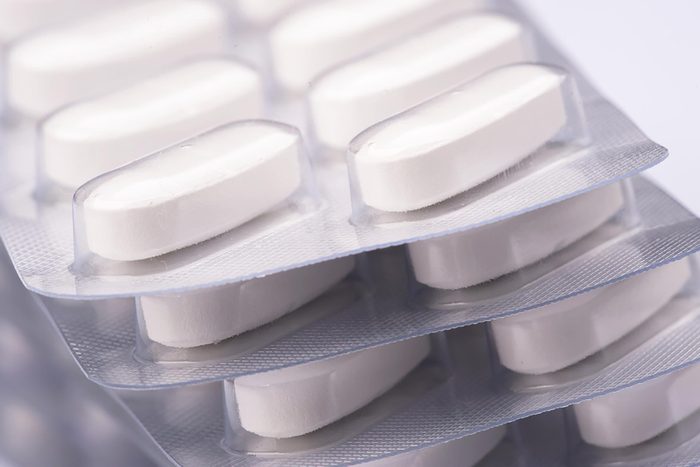
Will a generic drug be as effective as a name brand?
Being sick and paying outrageous prescription prices is a double whammy nobody wants, but will lower-cost generic drugs be as effective as the trusted name brand? According to Chan, the FDA requires that generic medicines work the same way as the brand name drug. Dr. Leavey agrees. “There may be differences in the way the pill or capsule is constructed, and this may lead to individual variations, but for the majority, there will be no problem,” says Leavey. However, there are some specific instances when a brand name product is best, he says. Ask your doctor if a generic med is right for your condition.
Next, find out hope to cope with medication side effects.

