
Heart disease is a leading cause of death
In Canada, about 12 adults die from heart disease each hour, making it the second leading cause of death nationally.
Still, heart disease is often preventable. So what accounts for such statistics?
A number of factors, says Salim Hayek, a cardiologist at the Michigan Medicine Frankel Cardiovascular Center at University of Michigan in Ann Arbor. “While aging is the major driver of heart disease, there are other important lifestyle factors that contribute, including smoking and the obesity epidemic.”
Heart disease doesn’t always cause symptoms. And even when it does, the symptoms can be subtle—like fatigue or shortness of breath that you may pass off as being out of shape.
Other times, heart disease is glaringly evident with heart attack symptoms such as chest pain, shortness of breath, lightheadedness, upper back or neck pain, or pain in one or both arms. (Never brush off these symptoms and call 911 immediately.)
(Related: What Causes Heart Disease? 9 Things Doctors Need You to Know)

What is heart disease?
Cardiovascular disease is a broad term that refers to a number of conditions and problems that affect the heart and blood vessels. Those include coronary artery disease, arrhythmias, high blood pressure, congenital heart defects, peripheral artery disease (a clogging of the arteries in other parts of the body, like the legs), and stroke.
While the term “heart disease” technically includes a number of conditions that affect the heart muscle, it’s often used as shorthand for the most common type, which is coronary artery disease—or a clogging of the blood vessels that supply the heart muscle with blood.
Here’s what you need to know about the different types of heart disease, including symptoms and causes, as well as heart disease prevention tips from leading cardiologists.
(Related: 6 Things You Probably Don’t Know About Heart Health)

Types of heart disease
Coronary artery disease
Coronary artery disease (CAD), also known as ischemic heart disease, accounts for about two in 10 deaths in adults under age 65, according to the Centers for Disease Control and Prevention (CDC). Coronary artery disease is the formation of fatty plaques or deposits in the blood vessels that supply the heart’s muscle.
The plaques can grow and cause partial or total blockages of blood flow in the heart’s arteries. If not enough oxygenated blood reaches your heart, you may have angina, a specific type of heart-related chest pain. If the blood supply is dramatically reduced or totally cut off, a heart attack occurs.
During a heart attack, the heart continues to beat, but a reduction of blood to the muscle results in tissue dying—although prompt treatment can help reduce the damage.
Some people with CAD might not even know they have the disease until they experience chest pain or a heart attack. That’s because there are no other symptoms or they’re mild and easy to dismiss.
Symptoms of coronary artery disease
- Shortness of breath
- Pressure, heaviness, or tightness in the chest
- Chest pain behind the breastbone
- Chest pain at rest or eases with rest
- Pain that spreads to the arms, shoulders, jaw, neck, or back
- Weakness and fatigue
- Sweating
- Nausea
Symptoms of coronary artery disease specific to women
Women can experience different symptoms than men when it comes to CAD, Dr. Hayek says. “They may not report typical ‘chest pressure’ in response to decreased blood flow to the heart, but instead experience nausea, back pain, neck pain, abdominal pain, and malaise more predominantly.”
It’s also important to note that the average age for CAD in women is higher than in men. The average age is 73 for women and 70 for men, according to the Journal of Women and Aging.
Causes of coronary artery disease
The following may increase your risk of developing CAD:
- Smoking
- High LDL (“bad”) cholesterol, high triglyceride levels, and low HDL (“good”) cholesterol
- High blood pressure
- Sedentary lifestyle
- Overweight or obesity
- Diet high in saturated and trans fats
- Diabetes
- Family history of heart disease
- Men over 45
- Postmenopausal women
(Related: 15 Heart Attack Prevention Tips Every Woman Must Know)

Arrhythmias
Your heart depends on consistent electrical signals to regulate your heartbeat, and sometimes the signals go haywire. Most often, arrhythmias are triggered by stress, exertion, medications, or hormone imbalances.
The electrical signals might become too slow, too fast, or erratic. When that happens, the heart doesn’t beat properly.
Without a consistent heartbeat, the heart can’t effectively get blood to the lungs, brain, and other vital organs. “The severity of these can range from being a mere nuisance to causing strokes and sudden cardiac death,” says Dr. Hayek.
Symptoms of arrhythmias
- Palpitations
- Pounding in the chest
- Lightheadedness
- Dizziness
- Shortness of breath
- Chest discomfort
- Weakness or fatigue
Causes of arrhythmias
Arrhythmias can be caused by a number of factors, including:
- Coronary artery disease
- High blood pressure
- Changes in the heart muscle
- Valve disorders
- Electrolyte imbalances
- Excessive alcohol consumption
- Excessive caffeine consumption
- Injury from a heart attack
- The healing after heart surgery
- Congenital conditions
- Certain drugs
- Other medical conditions
(Related: 8 Causes of Exercise-Related Chest Pain Besides a Heart Attack)
Atherosclerosis
A “hardening of the arteries” is the more familiar way of referring to atherosclerosis. Healthy arteries have a smooth lining, and blood flows through them easily and without resistance. But when plaque begins to build up inside the artery walls, the passages become narrow, and blood can’t flow as easily as it should. Or the plaque can break or rupture, triggering the formation of a blood clot that can completely block blood flow.
If this blood clot breaks off and travels, it can causes a blockage—and a reduction in blood flow—in another part of the body. (If that happens in an artery in the brain, it’s known as a stroke.) The cause of CAD is atherosclerosis specific to the heart.
Another similar term that is sometimes used is arteriosclerosis. In general, arteriosclerosis is used to describe blood vessels that become thickened, stiff, and inflexible for a number of reasons, while atherosclerosis is one specific type.
Symptoms of atherosclerosis
Since plaque generally builds up slowly, most people don’t experience symptoms right away. Some people may not be diagnosed until after a heart attack or stroke. And others might experience symptoms once the plaque builds up. The symptoms and severity range from person to person depending on what artery is involved.
Atherosclerosis can occur in the arteries of the heart (where it’s known as coronary artery disease), the neck (where it can lead to strokes), and the arms or legs, causing peripheral artery disease. For example, a blocked artery in the leg may cause cramping and circulation problems in the legs. Plaque buildup in the neck, however, causes stroke symptoms such as face drooping and vision problems. And this damage to the blood vessels can cause other problems, like erectile dysfunction.
Causes of atherosclerosis
Plaque causes the hardening of the arteries. Since plaque is formed from cholesterol, fat, and calcium, avoiding a diet high in saturated fat, trans fats, and salt can help lower the risk.
High blood pressure, diabetes, and smoking can also contribute to atherosclerosis as they damage the artery walls’ inner workings.
(Related: 7 Supplements Heart Doctors Take Every Day)

Cardiomyopathy
Having a big heart is an admirable trait when it comes to your character, but not your actual heart. In cardiomyopathy, the heart becomes enlarged, thick, or rigid. And bigger isn’t better.
“Cardiomyopathy refers to abnormalities in the heart muscle itself, often leading to weakening of the heart muscle and heart failure,” says Dr. Hayek.
“There are various types of cardiomyopathies ranging from genetic, ischemic (caused by heart attacks), and valvular (caused by defective valves),” he says. As this disease progresses, the heart becomes weaker and can’t pump blood through the body or maintain a normal electrical rhythm.
Symptoms of cardiomyopathy
Some people never have symptoms, while others might experience some in the early stages. As the disease progresses and worsens, signs of heart failure can occur. Heart failure is a chronic condition where the heart is enlarged but struggles to pump enough blood to supply the body’s needs.
It can cause symptoms like fatigue and shortness of breath or trouble breathing, especially with exertion, as well as swelling and fluid accumulation in the lungs, legs, and feet.
Other symptoms include:
- Dizziness
- Lightheadedness
- Fainting during physical activity
- Irregular heartbeat
- Heart murmur
- Chest pain with physical exertion or after heavy meals
Causes of cardiomyopathy
Cardiomyopathy can be inherited or developed. Certain risks that contribute to cardiomyopathy are:
- High blood pressure
- Viral infections
- Muscle disorders, like muscular dystrophy
- Certain medications
- Coronary artery disease
- Alcohol abuse
- Cocaine or methamphetamine
- Congenital or genetic types
(Related: 25 Heart-Health Secrets Cardiologists Want You to Know)

Valvular heart disease
The heart has four chambers. Each one has its own valve that acts as a gatekeeper, opening and closing the valve to move blood in the right direction every time the heart beats. When one or more heart valves fail to open and close properly, it can cause serious heart issues.
“Valvular heart disease refers to abnormalities in the heart valves,” Dr.Hayek says. “These can be tight (valvular stenosis) or leaky (valvular regurgitation), and can often lead to cardiomyopathy, heart failure, and arrhythmias.”
Symptoms of valvular heart disease
People with mild to moderate valvular heart disease may not realize they have it, as sometimes there aren’t symptoms. For those who do experience symptoms, these are the most common:
- Significant fatigue
- Pain in the abdomen from an enlarged liver (in tricuspid valve malfunction)
- Chest pain
- Fast, fluttering heartbeat
- Trouble breathing or shortness of breath
- Low or high blood pressure
- Dizziness, lightheadedness, or fainting
- Difficulty walking short distances
- Swollen legs, ankles, or feet
- Can only sleep in a sitting position
Causes of valvular heart disease
All heart valve disease types are more common with age because the valve flaps can become lined with calcium deposits that make them thicker and stiffer.
Other causes of valvular heart disease include:
- Congenital heart defects
- Endocarditis, an infection in the heart
- History of a heart attack
- Rheumatic heart disease
- Degenerative calcification
- High blood pressure
- Diabetes
- High cholesterol
(Related: How a Cardiologist Suggests You Manage Your Heart Attack Risk)
Heart infections
Myocarditis and endocarditis are heart infections caused by bacteria, parasites, or viruses—including Covid-19. Myocarditis causes inflammation of the muscular layer of the heart wall, while endocarditis targets the inner layer of the heart or the heart valves.
They can cause temporary or long-lasting damage to the heart. People with myocarditis and endocarditis might not notice symptoms, or they are passed off as general fatigue or another illness.
Symptoms of endocarditis
- Severe headaches
- Seizures
- Drowsiness
- Confusion
- Sudden fever
- Vomiting
Symptoms of myocarditis
- Lightheadedness
- Fever
- Chills
- Chest pain or pressure
- Heart palpitations
- Chest congestion or coughing
- Joint paint
- Swelling in hands, ankles, and feet
- Skin rash
- Loss of consciousness

Diagnosing heart disease
“There are several tools that can be used to diagnose heart disease,” says Dr. Hayek. Your doctor will start with a personal and family history, ask about current and past symptoms, and schedule blood tests.
“Injury to the muscle of the heart can often be diagnosed through blood tests,” Dr. Hayek adds. Once those results come in, more tests may be ordered. That doesn’t necessarily mean you’re facing a grim diagnosis.
Remember, most heart diseases are vastly improved with healthy lifestyle choices. However, a diagnosis is essential to put a treatment plan in action.
Here are the more common noninvasive (no medical instruments are inserted into the body) and invasive (medical devices inserted in the body) tests to diagnose heart disease:
Noninvasive tests
- Cardiac computerized tomography (CT)
- Echocardiogram
- Electrocardiogram (ECG or EKG)
- Cardiac magnetic resonance imaging (MRI)
- Stress tests
- Event monitors
Invasive tests
- Coronary angiogram (catheterization)
- Biopsy
- Radionuclide ventriculography
- Electrophysiology study
(Related: I Had POTS Syndrome But Was Misdiagnosed With Anxiety)

Heart disease treatments
Treatment varies from person to person and depends on the type of heart disease you have and how advanced it is. Your treatment may include medications, surgery, invasive procedures, and/or lifestyle changes, such as eating a healthier diet, starting an exercise program, and stopping smoking. y
Implants like a pacemaker can help control arrhythmias or an implantable defibrillator can help avoid cardiac arrest, which is when the heart stops beating.
What you can and can’t control with heart disease
While heart disease can lead to heart attacks, you have more control than you may think to avoid one.
“The INTERHEART study showed 90 percent of global risk of heart attacks is predicted by modifiable risk factors,” says Janet Wei, MD, a cardiologist at the Smidt Heart Institute at Cedars-Sinai in Los Angeles.
That means heart attacks are potentially preventable by addressing risk factors such as smoking, diabetes, hypertension, nutrition, and exercise, Dr. Wei says.
Still, she adds that there are some risk factors we have no control or less control over such as genetics and psychosocial factors.
Genetic factors
“Our genes predispose us to the development of heart disease, to the risk factors for heart disease, and to differences in how we respond to heart-protective medications,” says Dr. Wei.
Whether you’re male or female can also influence your cardiac risk, she adds. But don’t be too quick to blame your parents for a heart condition.
“The vast majority of cardiac conditions are not genetic, and how family history impacts the risk of an individual is quite complex,” says Dr. Hayek. “The best approach is to be aware that certain forms of cardiovascular disease could be genetic. Let the cardiovascular specialist know of any concerning family history.”
Psychosocial factors
While some psychosocial factors aren’t totally out of our control, they can make heart disease more challenging to manage or get the proper care. According to Dr. Wei, these include low socioeconomic status, stress—both at work and in your personal life—structural racism, anxiety disorders, and depression.
“Efforts to optimize resilience to stress, to address health disparities, and to promote health equity are important to help reduce the impact of these psychosocial factors on our heart health,” she says.
(Related: The Forces That Shape Health Care for Black Women)

Heart disease prevention
When it comes to heart disease, an ounce of prevention really is worth a pound of cure. Here are Dr. Wei’s top tips to help prevent heart disease:
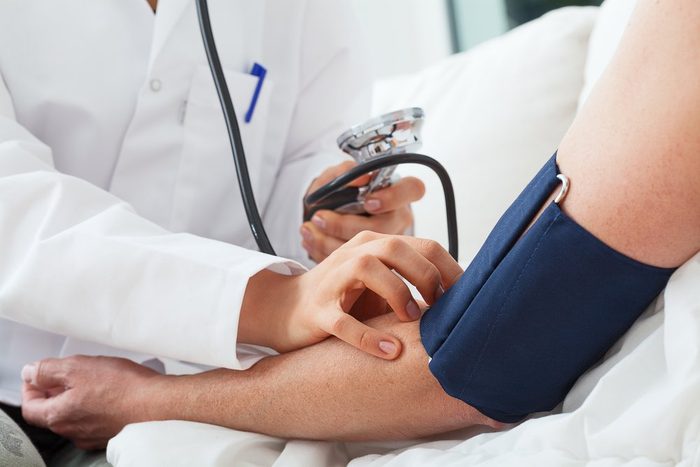
Know your numbers
“Check your blood pressure, body mass index (BMI), cholesterol, and fasting blood sugar level,” Dr. Wei says. “You can protect your heart by achieving ideal numbers early in life and maintaining these numbers for as long as possible.”
What’s ideal? “The ideal blood pressure is less than 120/80 mm Hg,” she says. “A normal BMI should be between 18.5 to 25 kg/m². Total cholesterol is 200 mg/dL, and fasting glucose should be less than 100 mg/dl.”
Get plenty of sleep
“Sleeping less than six hours a night is associated with a 20 percent increased risk of heart attack compared to sleeping six to nine hours a night,” says Dr. Wei. “And healthy sleep habits can decrease your blood pressure, weight, and risk of heart failure.”
Stop smoking
“It is never too late to quit smoking,” says Dr. Wei. “Smoking cessation decreases your risk of death and heart attacks by half. By three years, your risk for a heart attack is similar to someone who has never smoked.” Ready to stop smoking for good?
Eat the rainbow
“Challenge yourself to eat fruits and vegetables of different colors each day as a part of every meal, whether it is fresh, frozen, cooked, baked, roasted, or blended,” says Dr. Wei. “Eating a wide variety of naturally colorful foods provides heart-healthy nutrition that is high in vitamins, minerals, antioxidants, and fibRE.”
Stay active
“As little as 15 minutes of physical activity each day can boost your life span by three years and lower your risk of heart disease,” says Dr. Wei. “Aim for at least 30 minutes of exercise daily, and this can be spread throughout your day. Walk in place, dance, or do jumping jacks while watching TV. If you have a desk job, stand up and stretch or take a short walk for five minutes each hour.” The Physical Activity Guidelines for Americans from the U.S. Department of Health and Human Services recommends 150 minutes of exercise per week.
This story was medically reviewed by Michael Spertus, MD.
