Are stroke symptoms different for women?
If you’re at risk for a stroke, one acronym could save your life: FAST, developed by the American Stroke Association (ASA), which stands for Face drooping, Arm weakness, Speech difficulty, and Time to call 911. But these aren’t the only or even most obvious stroke symptoms in women, says Cheryl Bushnell, MD, professor of neurology at Wake Forest Baptist Medical Center, adding that more research is needed to determine why the difference exists. Women do have unique risk factors—hormones, for instance—and the risk of stroke is very real. One-third more women than men will die of stroke in Canada, reports the Heart & Stroke Foundation of Canada (heart disease and stroke are the cause of death for one woman every 17 minutes). Here are some symptoms and risk factors that are more common in women:

Fainting or seizures
You might be tempted to minimize a fainting spell, but maybe you shouldn’t: Women tend to suffer strokes to the back of the brain more often than men, says Diana Greene-Chandos MD, FNCS, assistant professor of neurosurgery and neurology at The Ohio State University Wexner Medical Center. Known as posterior circulation strokes, they cut off “blood flow to the occipital lobes, brainstem, cerebellum, and part of the temporal lobe. The top of the brainstem is where the consciousness center lies,” Dr. Greene-Chandos says, and cutting blood flow to this part of the brain can lead to fainting. She notes, however, that fainting “could also be related to a hyperventilation response to any type of stroke, as a fear response,” and that seizures, another of the stroke symptoms in women, can also be confused with a loss of consciousness.
Difficulty breathing
Although women would think chest pain and shortness of breath are signs of a heart attack, it could be a stroke. “This is consistent again with posterior circulation problems from the bottom of the brainstem where the respiratory drive centers lie,” says Dr. Greene-Chandos. Early recognition of stroke signs is crucial, says Kathryn Rexrode, MD, chief of the Division of Women’s Health, Brigham and Women’s Hospital. “It is important to get prompt emergency care if you are experiencing stroke symptoms since some strokes can be stopped by use of thrombolytic, or clot-busting, drugs,” she adds.

Hiccups
According to a survey from Dr. Greene-Chandos and colleagues at The Ohio State University Wexner Medical Center, only ten percent of women surveyed knew that hiccups, combined with atypical chest pain, are among the early stroke symptoms in women. “Hiccups are consistent with posterior circulation problems from the brainstem,” Dr. Greene-Chandos says. “The brainstem holds swallowing and the drive to breathe,” along with other functions.
Related: 6 Things You Probably Don’t Know About Heart Health

Sudden behavioral changes or agitation
Women are half as likely to report a non-traditional stroke symptom compared to men, according to findings from the University of Michigan; the most common of these symptoms was a shift in a woman’s mental state. Dr. Greene-Chandos believes this could be consistent with a posterior circulation stroke, which could target areas responsible for memory and personality. However, the frontal lobe is also tied to personality, so behavior changes “could be due to a frontal lobe stroke as well,” she says.

Nausea or vomiting
A stroke in the cerebellum can also lead to dizziness, nausea, and vomiting, Dr. Greene-Chandos says. “This is consistent with posterior circulation problems from either the brainstem or the cerebellum.” It can also be seen in intracranial hemorrhage-type of strokes as well, she says, in which a bulging blood vessel (an aneurysm) bursts and causes bleeding into the brain.
Related: This Common Type of Stress Can Give You a Heart Attack

Hallucination
While changes in your vision are a relatively common sign, according to the National Stroke Association, women’s visual symptoms may include hallucinations. Your occipital lobes—”the powerhouse of interpretation of visual input,” Dr. Greene-Chandos says—can be damaged by posterior circulation problems.
Related: How to Manage Your Heart Attack Risk, According to a Holistic Nutritionist

Early menopause or early menstruation
Starting either one of these life changes ahead of schedule can alter a woman’s risk, according to Dr. Rexrode’s research. Starting menstruation before ten years of age or menopause before 45 can indicate a higher risk of a stroke. “During the years that woman is menstruating, she produces higher levels of estrogen and other hormones,” Dr. Rexrode says, and it may be that the shortened exposure to these hormones bumps up risk—but researchers are still studying this.
Related: 8 Easy Ways to Clean Up Your Diet for a Healthier Heart

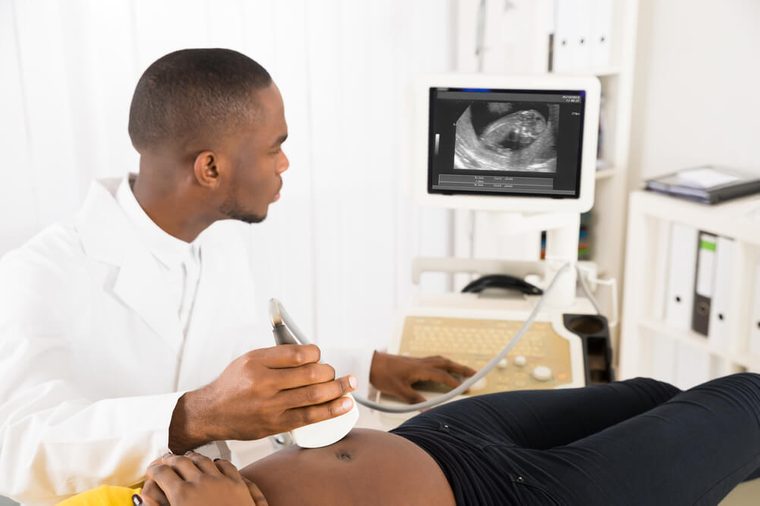
Some pregnancy complications
Preeclampsia—dangerously high blood pressure during pregnancy—can raise your stroke risk later on in life. So can the pregnancy complication of gestational diabetes. Preeclampsia is a sign of stress on the circulatory system, and it can predict the risk of developing high blood pressure later in life, explains Dr. Bushnell. “Also, gestational diabetes is associated with an increased risk of diabetes—both hypertension and diabetes are very important stroke risk factors.” That’s why the ASA’s new stroke guidelines for women, authored by Dr. Bushnell, recommend that doctors consider a patient’s health during pregnancy. Dr. Rexrode notes that pregnancy itself also boosts stroke risk.
Multiple miscarriages
Unfortunately, unsuccessful pregnancies may also be a predictor of stroke risk, if the miscarriages were due to a clotting disorder, according to the American Stroke Association. “The clotting factors increase the risk of developing clots in the heart or in the blood vessels of the brain, both of which can lead to stroke,” Dr. Bushnell says. Another sign of a clotting disorder is a history of clots in the legs, also called deep vein thrombosis (DVT).

Low levels of a key hormone
Dr. Rexrode’s research identified another stroke risk in women: low levels of DHEA (dehydroepiandrosterone). “DHEA, a hormone made by the adrenal glands, is used in the manufacture of other hormones including estrogens and androgens [male hormones],” she says. “It is not entirely clear whether low DHEA levels reflect some other underlying problem, or whether the effect on risk of stroke is through their influence on other hormone levels.”

Migraines with aura
These vicious headaches are more common in women. According to the American College of Cardiology, having migraines with the visual disturbances known as auras is a risk factor for stroke. Dr. Greene-Chandos points out that migraines are known to constrict brain blood vessels, and that could contribute to cutting off blood supply to the brain. “This increases the risk of stroke,” she says.

Autoimmune disease
Women are also more likely than men to have autoimmune conditions like lupus, Dr. Greene-Chandos says. Recent research from Spain has shown that autoimmune diseases can raise the risk of stroke and cardiovascular disease. The link may be inflammation, says Dr. Green-Chandos: “Autoimmune inflammatory conditions put women at risk for inflammation of the cerebral vasculature [blood vessels].”

Mental health and stress
Although the connection between mental health and stroke isn’t clear, scientists do know that stress is a risk factor for high blood pressure and cardiovascular problems—and women may be uniquely susceptible to stress, says Dr. Bushnell. A preliminary study from Harvard found that heightened activity in the amygdala, the area of the brain involved in the stress response, was associated with a greater risk of stroke.
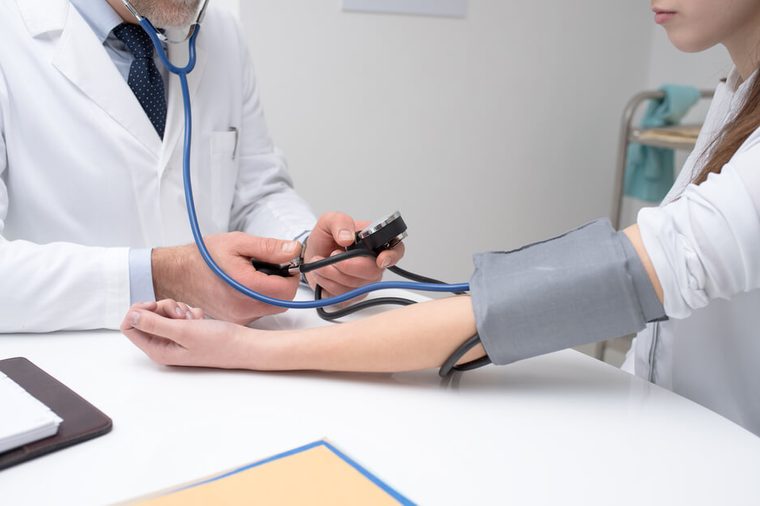
Irregular heartbeat
Officially known as atrial fibrillation (AFib), this symptom is particularly concerning as women age. According to the American Heart Association (AHA), women with untreated AFib have five times the risk of stroke. “Atrial fibrillation leads to blood clot formation in the heart, which can then break off and lodge in a blood vessel in the brain,” Dr. Bushnell says. For some reason, AFib stroke risk tends to be a bigger issue for women; the AHA/ASA guidelines advise that women over age 75 should be screened for AFib.
This story was originally published in April, 2018.

