It’s more common than people realize
Approximately one in 10 women of reproductive age suffers from endometriosis to some degree. That’s nearly two million women in Canada and more than 10 million women in the United States. “If all the women in the U.S. with endometriosis lived in one city, it would be the biggest city in the U.S.,” says Piraye Yurttas Beim, PhD, CEO and founder of Celmatix and board member for the Endometriosis Foundation of America. Learn about miscarriage and infertility.

Too few women are educated on the disease
Since painful periods are often considered to be a normal part of being a woman, many sufferers don’t realize that this monthly pain is a sign that they have endometriosis, explains Dr. Beim. In fact, in a recent survey conducted by her company, 37 percent of women said they hadn’t heard of endometriosis and don’t know what it means, while another 41 percent said they were somewhat familiar with it but still had questions about endometriosis and couldn’t describe it to a friend.

You’re not born with it
Because endometriosis is dependent on the presence of estrogen in the body, most girls don’t have it until they go through puberty—typically as early as age 10. “The painful symptoms can start even before a girl has gotten her period,” says Barbara Stegmann, MD, OB/GYN, reproductive endocrinology and infertility specialist at Aspire Fertility. “Additionally, the pain can be very debilitating at any age.”

It’s extremely difficult to diagnose
Even for specialists, endometriosis is one of the most difficult reproductive conditions to diagnose, which can explain why it goes unrecognized in most sufferers until age 32. “On average, women see four or more doctors for their pain before they are diagnosed with endometriosis,” says Dr. Stegmann. The main reason why is because the most efficient diagnostic tool is surgery. “Blood tests have not been very accurate and ultrasound or MRI do not usually show the lesions,” she adds. “The exception is when there is a cyst in the ovary, as this has a very characteristic appearance and the diagnosis can be made with ultrasound or MRI.”

It’s hereditary
Like most reproductive conditions out there, women who have sisters, mothers, or aunts with endometriosis are more likely to get it themselves. Additionally, women who have never had a child or have periods lasting longer than seven days are more at risk, explains Sherry Ross, MD, OB/GYN and women’s health expert at Providence Saint John’s Health Center in Santa Monica, California. “Severe acne as a teenager and certain pesticides have also been studied as a possible link to endometriosis.”
Related: Your Period Through the Decades — Here’s What Normal (And What’s Not)

It’s more common in certain ethnicities
For reasons that aren’t completely clear, indicates that endometriosis is most prevalent in women of Asian descent; Caucasian women have the second highest rate. Additionally, Dr. Ross points out that endometriosis is associated with other health problems that can be more common in women, such as asthma, allergies, multiple sclerosis (MS), hypothyroidism, chronic fatigue syndrome, fibromyalgia, and both ovarian and breast cancer.
Related: Could You Be At First For One of These Menstrual Disorders?

Doctors don’t know what exactly causes endometriosis
Although researchers believe genetics may play a role, the actual cause of endometriosis is unknown. That means there is little women can do to prevent the condition. “Many experts believe that keeping your estrogen levels low can help,” says Dr. Ross. “The birth control pill, regular exercise, avoiding excessive alcohol and caffeine all help keep estrogen levels low in your body and help reduce your risk.” Learn more about birth control options here.

Pain isn’t always associated with severity
While pain will vary from woman to woman, it’s not always a predictor of severity, according to experts. Doctors use a staging system to classify endometriosis, with stage 4 being the most severe. Nonetheless, experts say that women with stage 1 are sometimes more debilitated by their symptoms than those with stage 4; the staging system is more useful for rating infertility than as an indication of a patient’s quality of life.

It’s not always in the pelvic area
While most endometriosis is found in the pelvic area, Joshua U. Klein, MD, FACOG, chief medical officer and reproductive endocrinologist at Extend Fertility, explains that there are rare cases of endometriosis appearing in remote areas of the body such as the brain and lungs. “As endometrial tissue is responsive to hormonal stimulation, women who have endometrial tissue in their lungs can have monthly or cyclic problems such as a collapsed lung that occurs in concert with their menses. It’s known as ‘catamenial pneumothorax,'” he says.
Related: These Yoga Poses are Better for Pelvic Health Than Kegels
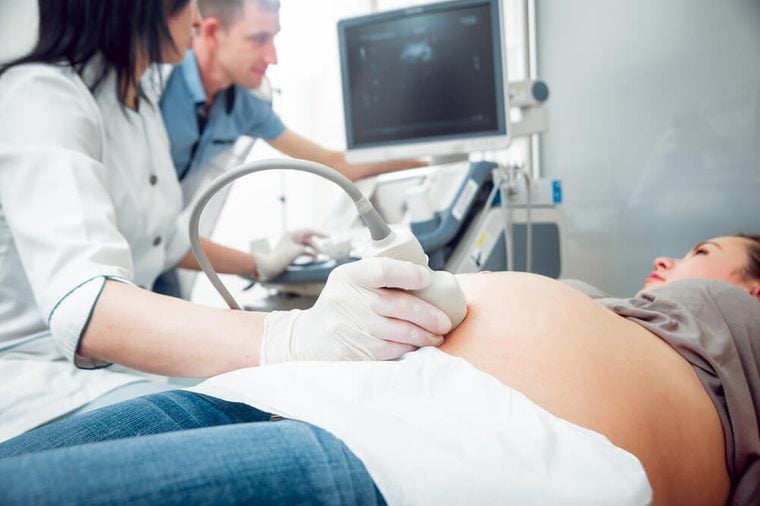
It’s a common cause of infertility
While not all women with endometriosis will experience infertility, endometriosis is one of the main causes: 35 to 50 percent of women diagnosed with endometriosis will have difficulty trying to conceive, according to one study. “For those with endometriosis, there are many different fertility challenges that can result—blockage of the fallopian tubes, damage to the egg supply (also known as the ovarian reserve), scar tissue, and adhesions that impact reproductive function and an overall hostile environment for sperm and eggs to flourish within,” explains Jennifer Hirshfeld-Cytron, MD, OB/GYN, director of Fertility Preservation at Fertility Centers of Illinois. “With surgery, some of these issues can be remedied and fertility treatment options such as in vitro fertilization, medically-stimulated cycles, and intrauterine insemination are commonly used by endometriosis patients with success.”

Pregnancy often comes as a relief
Aside from the fact that some women who have endometriosis often face infertility fears, pregnancy often provides physical as well as emotional relief from the condition. “With the uterus housing a growing child rather than building endometrial tissue to shed each month during a period, the cause of unpleasant and painful symptoms is absent,” says Dr. Hirshfeld-Cytron. “For this same reason, women find that endometriosis symptoms begin to diminish once menopause begins.” Prepare for this big life change by reading up on these silent symptoms of perimenopause.
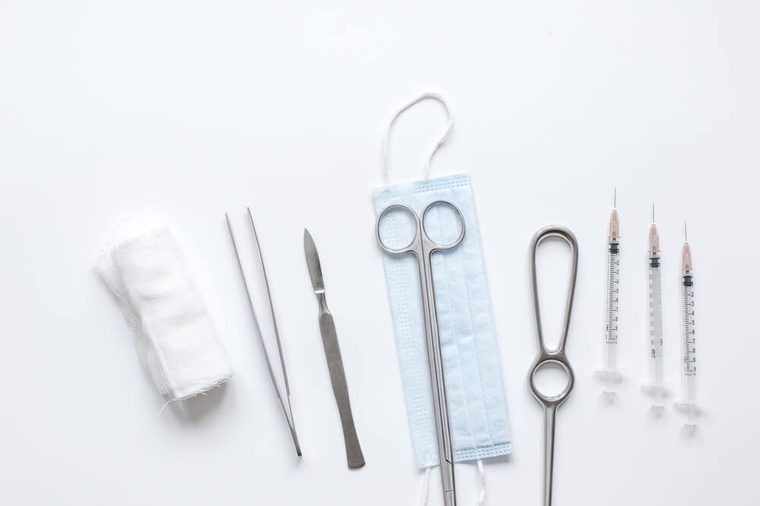
There is no cure for endometriosis
Science is still searching for a way to get rid of the condition. In the meantime, women can try multiple of treatment options, including medicinal and hormonal therapies, and even surgery. “Women with severe endometriosis may opt for definitive surgery with removal of the uterus and ovaries, although this removes the option to carry a child,” says Dr. Hirshfeld-Cytron. Drugs that suppress menstruation, such as hormone medications or birth control pills, can also help with symptoms, she says, but are not a cure.

Endometriosis can be emotionally and mentally debilitating
Numerous studies reveal that endometriosis can be emotionally devastating, especially since so many women struggle to find a diagnosis. In the meantime, they’re often told that their pain is all in their head, or they’ll get bad information and be prescribed unhelpful treatments.
Related: Julianne Hough Shares Her Struggle with Endometriosis on Social Media
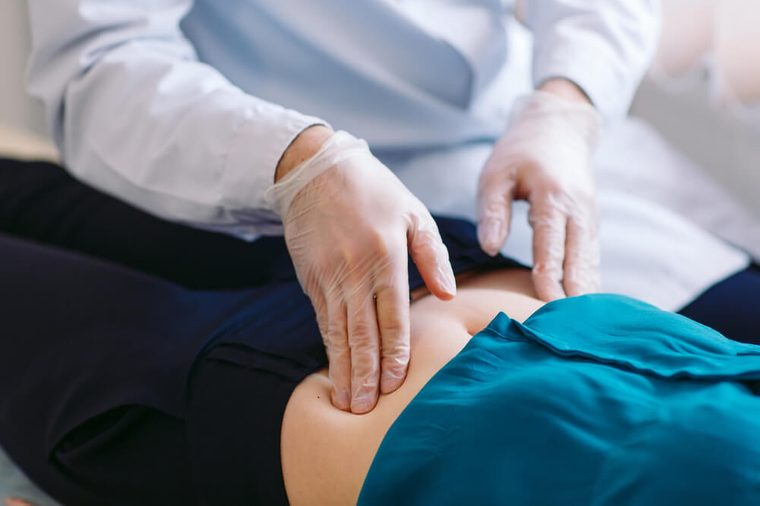
Sufferers should see a specialist
If you are concerned that you have endometriosis, make sure you see someone who specializes in this disease. “Reproductive endocrinologists have training in the diagnosis and treatment of endometriosis, and many general practitioners have a lot of experience with the disease,” says Dr. Stegmann. “If you are having pelvic pain and don’t feel that anyone has looked for endometriosis, don’t be afraid to seek out a specialist.”

There are still unanswered questions about endometriosis
In 2016, endometriosis received $10 million in federal research funding. While that might sound like a lot, Dr. Beim puts things in perspective by noting that, anthrax, which had zero cases in the US in 2016, received $51 million that same year. “Federal research dollars for endometriosis amount to approximately $1 per year for each woman affected by the disease,” she says. Worldwide, the average cost of endometriosis is about $10,000 per woman, per year, primarily due to lost work productivity and direct health care costs, Dr. Beim points out. That translates to an overall cost per year of about $3.7 trillion, roughly equivalent to the GDP of Germany.
Related: Could Your Beauty Products Be Sabotaging Your Fertility?

