What is fibromyalgia?
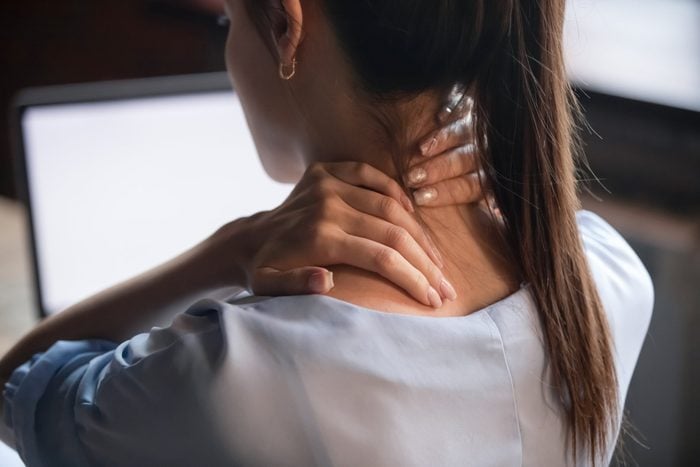
Fibromyalgia is a medical puzzle: The symptoms are so common that it’s both underdiagnosed and misdiagnosed for similar problems. “Fibromyalgia is a disorder of the central nervous system that causes widespread pain,” says Seth Lederman, physician, scientist, and co-founder and CEO of Tonix, a pharmaceuticals company. “Most often people with this long-term illness are fatigued, have sleep problems, and are plagued with tenderness throughout the body, especially in the neck, shoulders, arms, back, hips, and legs.”
While the cause of fibromyalgia is unclear, doctors believe the condition may run in families. But because there are no blood tests or scans to easily diagnose it, many physicians have trouble detecting the disorder. Here are some common conditions your doctor may consider before diagnosing you with fibromyalgia.

Arthritis
Although both conditions are indicative of widespread pain and constant fatigue, arthritis and fibromyalgia have their differences. “Many people tend to think that fibromyalgia is an actual form of arthritis, but that is not the case,” says Michael H. Lowenstein, PhD, medical director at the Waismann Method Opioid Treatment Center in southern California. “While it is characterized by pain, fibromyalgia does not cause tissue inflammation nor does it physically damage the body’s muscles and joints like arthritis is known to do.”
In the early stages of arthritis, this physical damage has not taken its course yet, so a patient only experiences the painful sensations, muscle stiffness, and exhaustion that are more in line with fibromyalgia. Only later when arthritic symptoms have further developed can a physician rule out fibromyalgia by taking an X-ray. (Find out what doctors do to prevent arthritis.)

Multiple sclerosis
While multiple sclerosis (MS) and fibromyalgia are two very different diseases, there are similarities—particularly the chronic pain that affects most of the entire body. “MS is a neurological condition that attacks and destroys the myelin, or protective coating, surrounding our body’s nerves,” says Anca D. Askanase, MPH, rheumatologist and associate professor of medicine at Columbia University Medical Center. “Once the damage is done to the outer layer of the nerves MS attacks the nerves themselves, causing the individual to lose sensation throughout their body.”
Although the symptoms are relative to the amount of damage MS has done to the nerves, it is common for sufferers to experience chronic pain throughout. “Symptoms of MS that may be different to fibromyalgia include difficulty walking, blurred eyesight, and slurred speech,” says Lederman. Unfortunately, both conditions are equally difficult for doctors to diagnose. “Most physicians can only come to a diagnosis of fibromyalgia or MS after they’ve ruled out other possible causes,” says Nathan Wei, MD, board-certified rheumatologist.

Lupus
This condition—in which the body’s immune system goes haywire and begins attacking healthy tissue—triggers symptoms such as fatigue, muscle pain, and soreness that’s often made worse by difficulty sleeping. “Lupus is an autoimmune disease affecting at least 1.5 million Americans that can cause damage to pretty much any area of the body, from the epidermis to the joints and even the body’s inner organs,” says Lederman. “Lupus patients may experience similar tiredness and soreness to those suffering from fibromyalgia, but some of the first signs of lupus are clearly different, including a rash across the face that worsens in the sun, difficulty breathing, kidney failure, stroke or even a heart attack.”
To help detect the difference, doctors likely will conduct a blood test that measures the patient’s level of antinuclear antibodies. Most of the time this test will show up positive if the patient has lupus, and is followed up by other special tests to come to a more definite diagnosis.

Chronic fatigue syndrome
Because there is no single lab test for chronic fatigue syndrome, and the fact that its symptoms—fatigue, memory loss, muscle and joint pain, trouble sleeping, etc.—are similar to many other conditions including fibromyalgia, doctors have a difficult time diagnosing it. “For your doctor to come to a CFS diagnosis, a patient must be suffering from constant fatigue for at least six months, as well as experience other key symptoms,” says Wei.

Depression
Anyone who’s ever battled even a temporary bout of this mentally exhausting and deteriorating disorder knows it’s serious. But for those suffering from depression on a persistent basis, they may wonder if there may be something more to their diagnosis. “One of fibromyalgia’s key symptoms is depression, so it’s not uncommon for a person to think they may have fibromyalgia after months or years of experiencing the debilitating effects of depression,” says Lowenstein. “So it’s even more confusing for patients to know that the two disorders can occur congruently.” If you know you’re suffering from depression, but are not sure fibromyalgia could also be an issue, talk to your doctor about monitoring your symptoms. (Suffering from depression during Covid-19? Read up on these mental health tips from therapists.)
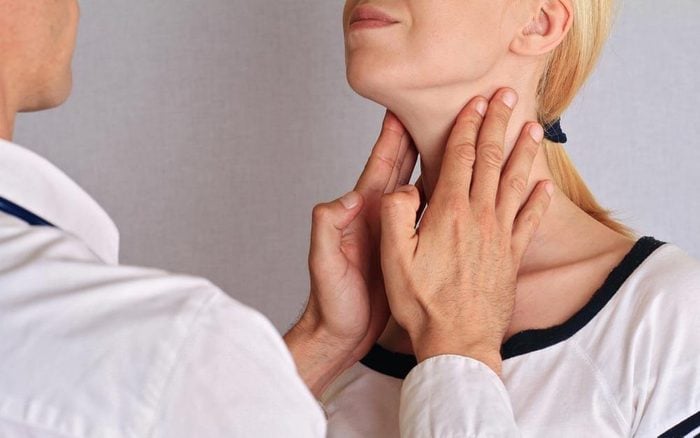
Hypothyroidism
This is a condition caused by an abnormally low amount of activity in the thyroid, the gland in your neck responsible for controlling your body’s metabolism. Due to an underproduction of hormones, a person experiences low energy, unexplained weight gain, greater sensitivity to cold, slow heart rate, and depression, among other symptoms. “Many of the symptoms of hypothyroidism coincide with those of fibromyalgia, so it can be difficult to differentiate the two just by analyzing symptoms,” says Wei. Your doctor can do a blood test to see if your thyroid hormone levels are healthy. (Plus, here’s what doctors want you to know about thyroid problems.)

Polymyalgia rheumatica
Yes, this also has “myalgia” in its name, but this mysterious condition also has similar symptoms to fibromyalgia. Polymyalgia rheumatica, commonly referred to as PMR, triggers aching and stiffness throughout the body, and just like fibromyalgia, it doesn’t often cause physical symptoms that could show up on an X-ray. Although the source of PMR is unclear, it appears to be an autoimmune disease. “In addition to chronic pain, PMR is known to cause trouble sleeping and achy joints,” says Lederman. “One key differentiator from fibromyalgia is that PMR is most common in adults over the age of 50—most often affecting those in their 70s and 80s.”
If you are older than 50 and are experiencing these symptoms, ask your doctor to monitor you for PMR. “While it’s hard to diagnose PMR, your doctor can test your blood for high inflammation, which is usually a sign of the condition,” says Lederman.
Next, check out these strange skin symptoms that could be a sign of a serious disease.
