
How much do you know?
According to the Canadian Dermatology Association, psoriasis is a common chronic inflammatory skin condition that involves red elevated patches and flaking silvery scales. It affects as many as one million Canadians and 80 million people worldwide. Lesions may be painful and itchy, and can appear anywhere on the body, but most commonly occur on the hands, knees, elbows and scalp, says Dr. Melinda Gooderham, a dermatologist at the Skin Centre for Dermatology in Peterborough, Ont. Psoriasis lesions occur as a result of the skin thickening at an abnormally fast rate. While psoriasis can be somewhat controlled, someone with the condition may experience flare-ups which disappear before another episode occurs.
Here are four things you should know about psoriasis, even if you don’t have the condition yourself.
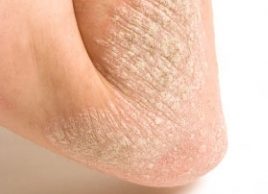
1. It’s not contagious
For someone who suffers from psoriasis, the condition isn’t only physical, but impacts him or her emotionally as well. “The number one complaint I hear is that other people [who don’t have psoriasis] see someone with it and think they’re contagious,” says Dr. Gooderham. “But it’s not a contagious condition.”
Since psoriasis is a visible condition and often occurs on parts of the body that aren’t always covered by clothing, people with psoriasis may have to deal with intruding looks or questions about their condition. Renae Addis, a former dancer who lives in Mississauga, Ont. says her psoriasis diagnosis was difficult due to the physical and emotional impact it had on her life. “I grew up on a stage and had always been really confident, but suddenly I felt very uncomfortable in public,” she says. At one point, Addis says her body was about 70 percent covered with psoriasis lesions. Having a moderate to severe form of psoriasis made it hard for her to continue being as active as she once was.

2. It most commonly occurs in adulthood
Psoriasis occurs equally among men and women and across different races, according to the Canadian Dermatology Association. “We also know there’s a genetic predisposition for it,” says Dr. Gooderham. “If you carry the gene, there’s usually a trigger that causes it to manifest, whether it’s stress or an infection.” However, says Dr. Gooderham, “only about one-third of patients know someone in their family with the condition, and there are approximately 20 different genes.”
Psoriasis could be triggered at any time from childhood to adulthood, but it most commonly occurs between the ages of 30 and 50.

3. Stress is a major contributor
Stress is the number one trigger, says Dr. Gooderham, because psoriasis is believed to be an immune system problem. Addis was diagnosed with the condition shortly after the birth of her daughter and says that stress was a big factor for her. She says her psoriasis was at its worse during that stressful time in her life.
Other contributing factors include local injury to skin, systematic infections and the use of certain medications.

4. There is relief
While the harsh winter weather can take a toll on anyone’s skin, people with psoriasis are particularly at risk for dry skin. Not to mention, psoriasis conditions can escalate in cold weather.
“The winter months are very difficult because having my psoriasis flare up is always in the back of my mind,” says Addis. “I have to make sure I moisturize well every day and keep my skin as healthy as possible.
Dr. Gooderham agrees that moisturizing every day is a good way people with mild psoriasis can keep the condition under control. “Having a humidifier in the house may also help,” she says.
Other treatment options include topical steroids and those in pill form, says Dr. Gooderham. Light therapy is also used to treat psoriasis. A physician or physiotherapist may give Narrow Band UVB phototherapy treatment, which is different from a tanning bed, says Dr. Gooderham. Those suffering from moderate to severe psoriasis may respond better to treatments such as oral retinoids or biologics.
If you think you may have psoriasis, see your doctor to get a proper skin diagnosis and determine the proper treatment plan for you.
Related:
• Psoriasis
• 7 strategies to soothe or prevent dry skin
• 5 reasons you skin is dry
