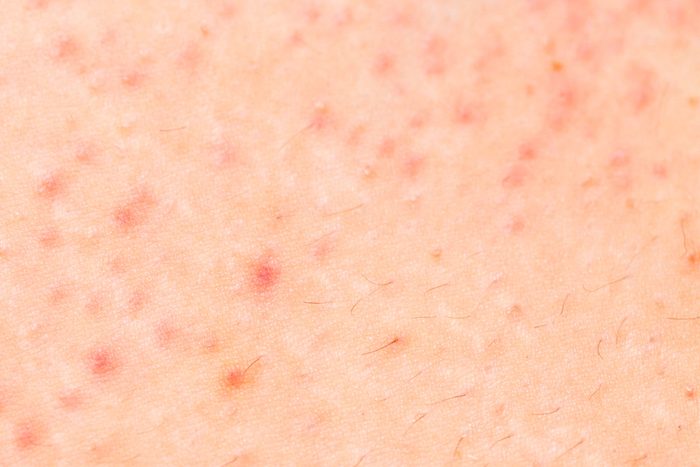
Rosacea
Rosacea is a chronic, inflammatory disorder often confused with acne. “While there are multiple types, the two most common include redness of the cheeks (flushing) and an over-abundance of little visible vessels on the cheeks, as well as acne-like bumps generally more in the mid face,” says New York City dermatologist Dhaval G. Bhanusali, MD. Unlike acne, rosacea is commonly triggered by histamine-related response and by spicy foods, caffeine, and alcohol. Treatments usually combine dietary and lifestyle changes, prescription topicals, and switching to non-irritating skin-care formulas.
Folliculitis
Folliculitis (a common summer skin problem) is an inflammation of the hair follicles, characterized by tiny, red pimples, which may be come filled with pus (resembling whiteheads). They can also be itchy or painful, or in more severe cases become crusty sores. They can appear anywhere on the body—particularly areas where friction is common, like the thighs, butt, neck, and armpits. (This woman even got folliculitis from her sweaty workout leggings.) According to New York City dermatologist Francesca Fusco, MD, folliculitis can be caused by bacteria and comes in several versions. Some examples include bacterial folliculitis, also known as barber’s itch because it tends to affect men’s beard area, and pseudomonas folliculitis, aka hot tub itch because the responsible bacteria is most commonly found in warm contaminated water. Mild cases of folliculitis can be treated with non-prescription benzoyl peroxide- and salicylic acid-based cleansers, wipes, and creams. More severe cases may require oral antibiotics. For folliculitis that involves a yeast infection, there are anti-yeast cleansers; often a prescription-strength antifungal medication may be required.
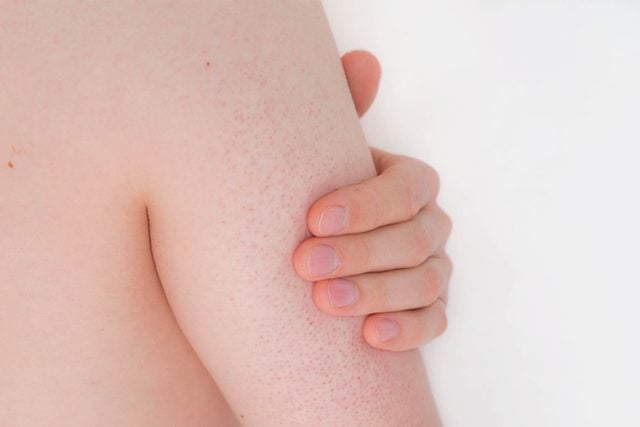
Keratosis pilaris
Keratosis pilaris is a chronic skin condition, marked by rough (red, white, or skin colored) bumps—usually on the upper arms and legs—that can feel like sandpaper. According to Dr. Bhanusali, these tiny bumps are caused by an abnormal amount of keratin that blocks hair follicles. While the condition is harmless, it can cause itchiness and dryness—moisturizers can help ease these symptoms. New York City dermatologist Debra Jaliman, MD, recommends treating keratosis pilaris with topical retinoids and creams containing salicylic acid and lactic acid, which work to remove dead skin cells and prevent clogged follicles. Don’t miss the things your skin can reveal about your health.
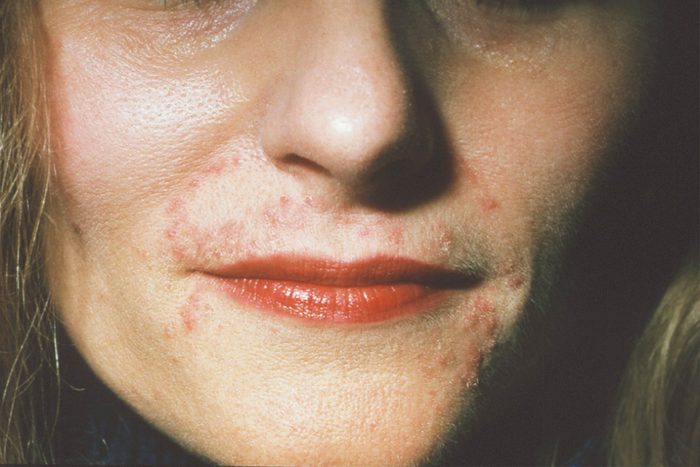
Perioral dermatitis
Perioral dermatitis is an inflammatory facial rash versus acne, which is bacterial—typically seen around the mouth. The most common cause is topical steroid use, but it can also be caused by fluoridation in toothpaste, explains New York City dermatologist Bobby Buka, MD. The recommended course of treatment is to discontinue all topical steroids (both prescription and OTC), heavy face creams, and fluorinated toothpaste—instead, opting for mild, non-irritating cleansers and lightweight, non-comedogenic lotions. Oral and topical antibiotics are an effective treatment option. The condition can also be caused by an overgrowth of skin mites and newer treatments target these organisms. These skin problems could be a sign of serious disease.
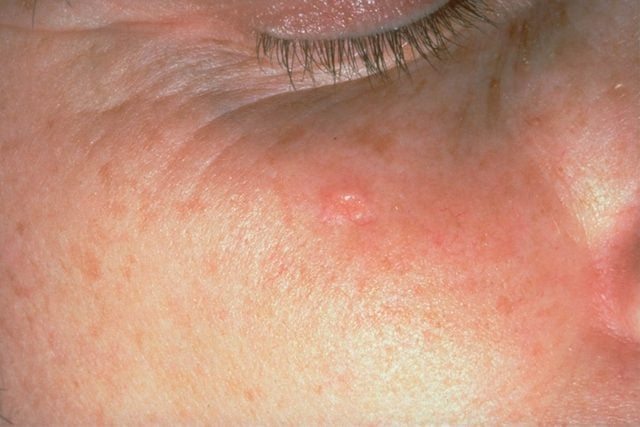
Sebaceous hyperplasia
Sebaceous hyperplasia is genetic condition characterized by flesh-colored, doughnut-shaped bumps that develop on the forehead, cheeks, nose, and chin. These lesions are actually enlarged oil glands (sometimes, you can even squeeze oil out of them). Sebaceous hyperplasia is benign. However some people choose to treat it for aesthetic reasons. One treatment option is called electrodessication, a device that delivers an electric current into the skin to help reduce the appearance of lesions. These myths about pores could be ruining your complexion.
Ingrown hairs
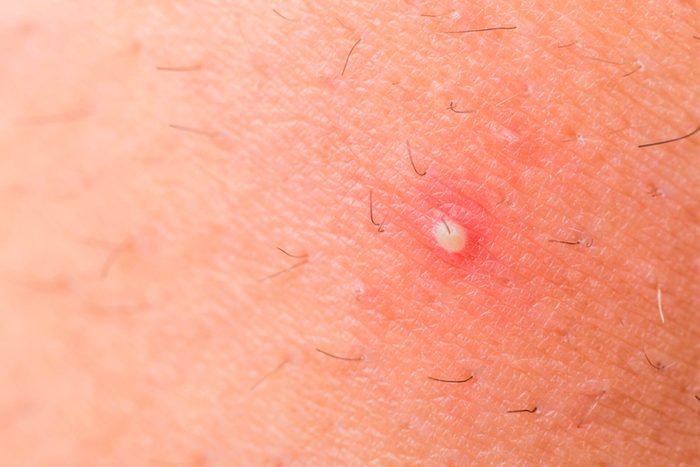
Ingrown hairs are hairs that have turned around and grown back into the skin, creating a raised bump. According to Dr. Fusco, they can look exactly like acne and present as white bumps, red bumps, or “underground” cysts. They are most common around the bikini and underarm zones in women, and in men, you’ll often see them on the chin, cheeks, and upper neck (the beard area). Resist the urge to pick, which can make them worse. Many times an ingrown hair will go away on its own, but if it doesn’t or it becomes infected you should make an appointment with your dermatologist. Depending on the severity, your doctor may recommend professional extraction or topical treatments, such as salicylic acid-based creams, cleansers, and pads, or retinoids. Here’s the truth about boils, cysts, ingrown hairs and 11 other skin mysteries.
Basal cell carcinoma
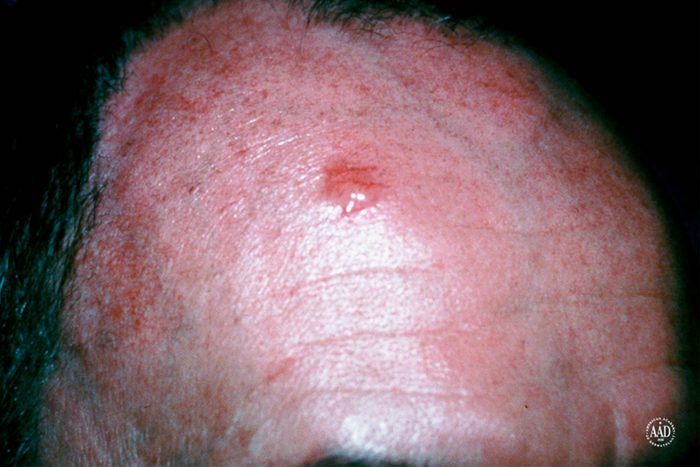
Basal cell carcinoma is a slow-growing type of skin cancer that derives from the base layer of the epidermis. It’s usually caused by excessive UV exposure, including sunlight and tanning lamps. Basal cells look like shiny, translucent or pink bumps with tiny blood vessels—and can often be mistaken for a persistent acne cyst. If you do have a lesion that doesn’t heal after a month or two, see your dermatologist for evaluation. Treatments include photodynamic therapy, Mohs surgery (a specialized type of skin cancer surgery to ensure clear margins, while minimizing the amount of skin removed), and tissue scraping. Next, discover which skin care ingredients you should be using all over your body.