Will I Need a 4th Dose of the COVID Vaccine?
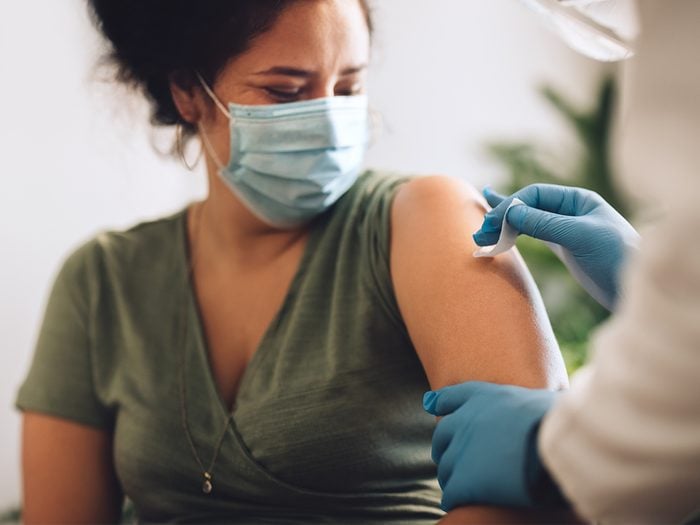
Our understanding of COVID variants and fourth doses is still evolving. Here is what we know so far.
With the Omicron variant surging across the country, more than 40 percent of fully vaccinated Canadian adults have received their booster—but many are already wondering if they should prepare for a fourth dose. These questions are fuelled in part by the COVID response in Israel, where a medical expert panel advising the Israeli government recommended fourth COVID-19 vaccine for all adults. Israel has already been providing fourth doses to anyone 60 and over since late last year.
Working as an internal medicine physician in Toronto, many of my patients have asked if they will eventually need fourth (and maybe even fifth) doses as the pandemic extends into its third year. Currently in Canada, anyone over the age of 18 is eligible for a third vaccine dose. Canada is also offering fourth booster vaccine doses to Canadians from high-risk groups, like residents of long-term care or those who are immunocompromised.
While it’s looking less and less likely the pandemic will come to a discreet end like we saw with SARS, it’s too early to determine if and how COVID will eventually become an endemic disease, meaning something we live with, like the flu or malaria.
It’s also too early to call if fourth doses or eventual seasonal ‘COVID boosters’ make sense for all Canadians. We don’t know yet how long three doses provide robust protection or if a new variant will arise that can evade the defence the vaccine provides.
Our understanding of fourth doses is constantly evolving, but here is what we know so far:
What’s the difference between a third dose and a COVID booster?
Before Omicron, the average person who received two doses of an approved COVID-19 vaccine was considered fully vaccinated.
Data quickly emerged that immunocompromised individuals, like transplant patients on anti-rejection drugs, had a lower antibody response with two doses and needed a third dose. These third doses were not considered boosters because these individuals needed all three doses for protection.
Last summer, we learned from Israeli data that a significant part of our antibody immune response wanes about six months after our second vaccine dose. When combined with winter Delta variant surges followed by the highly-mutated Omicron strain exploding in numbers, we started to see many more breakthrough infections in people with two doses of vaccine.
While two doses seem to provide enough protection to prevent recipients from needing hospitalizations and ICU admission, it is not enough to reduce transmission of Omicron, especially in higher risk indoor settings. Because of this, many experts are now thinking of Pfizer and Moderna COVID vaccines as three-dose vaccines, with all three doses needed to be ‘fully vaccinated.’ Many existing vaccines come in a similar three dose series, like the hepatitis B vaccine or the HPV vaccine.
With mounting evidence that three doses are better than two, the Public Health Agency of Canada plans to revisit the number of doses required to be considered fully vaccinated once more Canadians have had a third dose.
(Related: COVID-19 Vaccines Are Vital—And So Are These)
If this is a three-dose vaccine, why are some people now getting a fourth dose?
Canada, along with the U.S. and the U.K. are offering a fourth vaccine doses to people in high-risk groups and people who are immunocompromised. Individuals who are immunocompromised require more COVID vaccine doses to generate an immune response and COVID antibodies.
Because third doses were rolled out much earlier for high-risk individuals, their immunity is likely waning now, amid a surge in COVID cases. The hope is that four doses will induce a robust immune response to Omicron in those that are at the highest risk of complications, like long-term care residents, cancer patients, seniors who live in congregate settings and transplant patients.
Israel is one of the only countries that is already offering fourth vaccine doses to people over 60 since and is likely to start offering fourth doses more widely in the near future. On Jan. 3, Israel’s prime minister announced, based on the results of a small unpublished study of hospital staff, that antibody concentrations increased fivefold a week after a fourth vaccine dose. Though research is still ongoing, no data has been published yet and it remains to be seen what the value add of a fourth dose might be.
So, could we need another booster eventually?
It is possible, but not certain. There are many factors at play here. First, we need to better understand how much protection third doses give us and for how long. We also need to continue to collect any available data we have on fourth doses. It will take several months for researchers to know whether people who received fourth doses had more protection against infection, severe illness and hospitalizations than those with three.
Second, the amount of virus circulating in the community matters. If Omicron spread settles down and case counts decrease, we might not need the immunity boost from a fourth dose. But if a new variant emerges in the summer that is just as prevalent as Omicron, we may need that boost in immune response to curb the spread.
Israel has been several months ahead of us when it comes to vaccinating their population. Their data on fourth doses will hopefully help us understand if there is a benefit to larger sections of the population.
Why would we no longer need additional doses? It seems like that is where we are headed.
It has been notoriously difficult to predict the future during this pandemic. We simply don’t know exactly what will happen six months from now, whether it’s emerging variants or waning immunity.
Canada, along with the U.S. and U.K., is waiting for more data on waning immunity and effectiveness of vaccination in reducing hospital admission before it decides on offering a fourth jab to a wider group of people.
Researchers will be studying people’s antibody levels in the months following a third dose. While those levels are expected to drop in four to six months, the degree to which it will drop is unknown. If the drop is minimal to moderate, we may not need more doses.
There are also some new factors to consider, like how the outpatient antiviral treatment Paxlovid could impact hospitalizations and severe illness numbers as it becomes more widely available in Canada.
(Related: Everything You Need to Know About COVID Antiviral Pills)
Are we likely to see variant-specific boosters in the future?
In theory, COVID vaccines can be adapted and updated as variants emerge. But it still might not be fast enough.
Both Pfizer and Moderna made Beta- and Delta-specific vaccines, but it was found that the original vaccine had an equivalent response so there was no need to make a change. Pfizer is working on an Omicron-specific booster that could be ready for use as early as March. But with the speedy spread of Omicron, many people may experience an Omicron infection before the booster is ready. Also, third doses of the existing vaccine neutralized Omicron in preliminary studies, stunting the benefit of an Omicron specific booster.
If new variants continue to emerge, they could evade parts of our existing immune response from the vaccine, as we saw most recently with Omicron. At some point, more of the same vaccine may not be better and we may need to update the vaccine. We could also see the vaccine evolve in other ways. Moderna announced in the fall it was working on a new mRNA-based influenza vaccine that is combined with a booster COVID-19 dose.
We all hoped the pandemic would have ended by now. But the good news is that as the pandemic evolves, so have our tools to protect ourselves.
Dr. Seema Marwaha is a general internal medicine physician in Toronto and an assistant professor at the University of Toronto’s Department of Medicine. She is also the editor-in-chief of Healthy Debate.
Next: Could Protection from COVID Soon Be Available Through a Nasal Spray?




