
More than skin deep
Your next dermatologist visit could reveal important health information that you may not expect. “Skin is the window to your health,” says Wilma Bergfeld, MD, senior dermatologist in the department of dermatology in the Cleveland Clinic. Medical dermatologists are seeing more and more skin issues, especially related to immune system problems, including lupus, rheumatoid arthritis, and inflammatory bowel disease. In many cases, dermatologists might help discover conditions during routine visits—before a specialist would—which can ensure patients get treated in earlier stages of illness. Here are some important conditions your skin doctor has her eyes on.
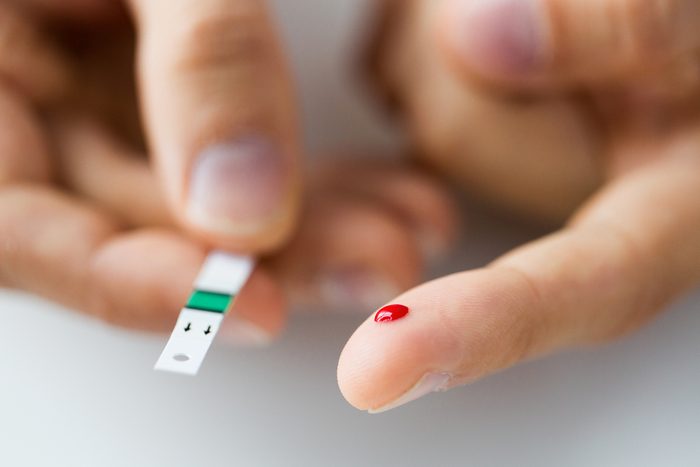
Type 2 diabetes
One of the skin diseases that can be a sign of pre-diabetes is acanthosis nigricans, a velvety thickening of the skin that occurs around the neck and in the underarms. Usually, patients with these dark patches don’t know they have diabetes when we see them, says Dr. Bergfeld. “In dermatology, they tend to be younger, so we pick up these cases early.” Skin tags are another sign, but they’re not an automatic red flag. Everybody gets skin tags under their arms every now and then, or in the groin area just from rubbing, according to the U.S. National Library of Medicine. That said, if you have multiple risk factors for diabetes, multiple skin tags, and acanthosis nigricans, your dermatologist might request a blood test.

Celiac disease
Super itchy clusters of blisters called dermatitis herpetiformis, which commonly occur on the elbows, knees, buttocks, and sometimes the scalp, are a clear sign of one condition: Celiac disease. It affects 10 percent of people with celiac—clearly, not everyone with celiac will have dermatitis herpetiformis. People who have this skin issue who don’t have any GI concerns are often shocked to learn they have celiac. And when they begin a diet free of gluten—the protein found in wheat, rye, and barley that triggers an immune system response in celiac patients—their skin gets better, too.

Rheumatoid arthritis
This inflammatory disease, which causes swelling and pain in the small joints of the hands and feet, can sometimes manifest in the skin. About 20 to 30 percent of rheumatoid arthritis patients can get subcutaneous (beneath the skin) lumps near an affected joint, according to Johns Hopkins Arthritis Center. “Thinning of the skin, a translucency of the skin on the back of the hands, or brittle nails may also be common signs of rheumatoid arthritis,” says Roshini Raj, MD, assistant professor of medicine at the NYU School of Medicine and co-founder of TULA skin care. (Here’s more on how to relieve rheumatoid arthritis symptoms.)

Lupus
A sunburn-like rash across the top of the cheeks is often an important clue for lupus, an inflammatory disease in which your immune system attacks the body’s tissues and organs. Patients with lupus may also have a red rash on their scalp and on areas of their skin that get a lot of sun exposure, such as the neck, the backs of the arms, and the upper back. Anywhere from 40 to 70 percent of lupus patients can find that sun exposure makes their disease worse, according to the Lupus Foundation of America.
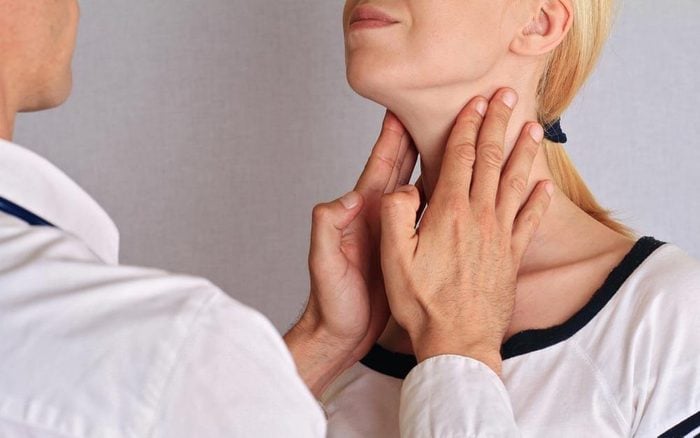
Thyroid disease
Chronic hives—those that last longer than six weeks—could be a sign of thyroid conditions like Graves’ disease or Hashimoto’s thyroiditis. Doctors aren’t sure why these conditions trigger hives, but suspect that the body develops antibodies against certain parts of the immune system called IgE receptors, which triggers the allergic reaction. (Learn how to tell if you have a hidden thyroid problem.)

Inflammatory bowel disease
Skin issues affect about five percent of people with inflammatory bowel disease, according to the Crohn’s and Colitis Foundation. This includes red bumps or nodules called erythema nodosum, enterocutaneous fistulas, and more. Another sign in colitis patients is something called pyoderma gangrenosum—ulcer-like lesions that tend to occur on the shins, ankles, and arms. They typically start as small blisters but merge to become deep ulcers. Many IBD-related skin conditions ebb and flow with disease flare-ups; when your GI tract acts up, so will your skin (Learn how a low-residue diet can help with inflammatory bowel disease.)
Hepatitis C
A number of skin disorders are associated with this liver disease, according to the Journal of the European Academy of Dermatology and Venereology. These include rashes like vasculitis and lichen planus—which each have very distinctive looks and patterns that a dermatologist should recognize.

Adrenal insufficiency
The adrenal glands—located just above the kidneys—are responsible for pumping out cortisol, a crucial hormone that helps the body respond to stress. Addison’s disease results when the adrenal glands don’t make enough cortisol, which can cause a diverse range of symptoms including muscle weakness and fatigue, weight loss and decreased appetite, low blood pressure and blood sugar, and more. Because symptoms of Addison’s disease can come on gradually and subtly, it’s often not diagnosed right away. One Addison’s symptom that’s a red flag for dermatologists is darkening of the skin; Dr. Bergfeld says it’s almost as if patients appear tan. Unexplained stretch marks in the skin are another sign.

Nutritional deficiency
“When patients come with hair loss or hair shedding, the most common triggers in women are nutritional and hormonal,” says Dr. Bergfeld. “When patients are on very restricted diets, they can have deficiencies in protein, zinc, vitamin D, and iron.” Other triggers for hair loss are hormonal problems such as androgen excess, in which an abundance of male hormones can cause a number of side effects, including hair loss on the head as well as increased body hair and acne.
Next, check out these dermatologist-approved face masks for acne.
