Top 10 Questions About High Blood Pressure, Answered
Have you been diagnosed with high blood pressure? We went straight to Canada’s experts for answers to the top 10 questions surrounding hypertension
Source: Best Health magazine, January/February 2016
1. How does high blood pressure inflict damage?
Just as a garden hose under too much pressure can bulge, blow out and blast too strongly onto delicate plants, blood flowing under too much pressure can weaken blood vessel walls, cause ruptures and damage delicate organs. That’s why hypertension is linked to strokes, heart attacks, aneurysms and eye and kidney damage. It also forces the heart to work harder, eventually contributing to heart failure.
2. What causes hypertension?
In about 95 percent of cases, there is no direct cause. This is called ‘essential hypertension.’ Obesity, lack of exercise, high alcohol and salt consumption, stress and family history are all risk factors. In addition, our blood vessels become stiffer as we age, raising our blood pressure. In the remaining five percent of cases, high blood pressure is brought on by another illness or medication known as ‘secondary hypertension.’ Causes may include thyroid disease, polycystic kidneys, adrenal gland problems and other illnesses. Medications and supplements that are known to raise blood pressure include oral contraceptives, cold and migraine medications, non-steroidal anti-inflammatory drugs for pain relief and herbal supplements like St. John’s wort.
Glycyrrhizic acid, a compound found in licorice-containing foods, candies, teas and herbal products, can have a dramatic impact. As little as half a cup of licorice tea a day may be enough to raise blood pressure. Ideally, your doctor will do everything possible to help you avoid unknown causes and exclude secondary forms of hypertension before making a diagnosis of essential hypertension.
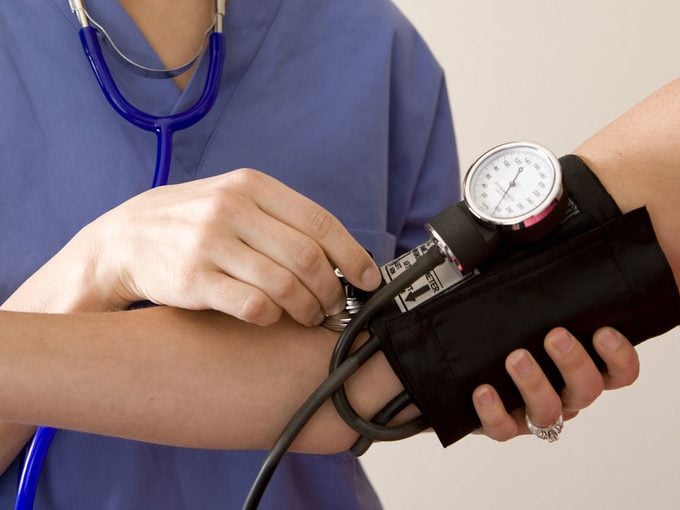
3. How is blood pressure measured?
Medical practitioners use a device called a sphygmomanometer. With a patient sitting still and her arm supported, a cuff is inflated around the upper arm at chest level. The doctor pumps up the cuff manually until the blood flow in the arm is stopped. Then, watching a dial or column of numbers, the doctor slowly releases the pressure until, with a stethoscope, he hears the first Korotkoff sounds, which represent the top number (systolic pressure). The pressure is released until all sounds disappear, representing the bottom number (diastolic pressure).
For the automatic method, a machine is used. Found at many pharmacies, these devices are usually of decent quality, but they’re not guaranteed to measure your blood pressure properly. ‘To get an accurate reading, you need a relaxed arm position, non-stressful circumstances, a well-calibrated machine and the right cuff size for your arm,’ says Dr. Frans Leenen, director of the Hypertension Clinic and Hypertension Research at the University of Ottawa Heart Institute. ‘These days, many people have a higher-than-normal weight, so the standard cuff doesn’t fit everyone.’
4. What do the two numbers mean?
The top number (systolic pressure) is the force exerted on your blood vessel walls when your heart beats and squeezes out blood. The bottom number (diastolic pressure) is the force on your vessels when your heart relaxes between beats.
Optimal blood pressure is considered at or under 120/80 mmHg (millimetres of mercury). If the pressure rises to over 140/90 mmHg, you have hypertension. If your numbers are in the higher part of the ‘normal’ range (130’139/81’89 mmHg), you still have an increased risk of stroke and other complications, says Dr. Norm Campbell, chair of the Hypertension Prevention and Control Initiative, funded by the Heart and Stroke Foundation of Canada.
‘There’s a misconception that high-normal is totally okay,’ he says. ‘Actually, both high-normal and hypertension are reasons for concern. The difference between them is that hypertension is the point where it starts to make medical sense to prescribe a drug ‘ despite the risks that drugs entail ‘ instead of trying to manage things with lifestyle factors alone.’
5. How often should your blood pressure be tested?
This matter is under debate, with no official right answer. However, if you are young and in good health, with none of the risk factors, and if your last reading was in the optimal range, then you could wait a few years before checking your blood pressure again. Otherwise, every six months or so should do the trick.
Dr. Campbell says that Canada is the best country in the world when it comes to diagnosing and controlling hypertension. Routine testing at doctor’s appointments plays a big role in this achievement, and workplace screening is helping to fill in the remaining gaps.
Other countries are doing a better job at prevention, though. Some have passed successful measures to restrict the amount of sodium in food, says Dr. Campbell (Belgium and Portugal, for example, have legislation that limits the amount of salt in bread). Our country, according to Dr. Campbell, has only an ineffective, voluntary salt-reduction system guided by Health Canada.
Dr. Leenen would like to see heart-damaging foods burdened with extra taxes, creating a revenue stream to subsidize the production of healthier options. At the end of the day, he says, our choices are determined by personal responsibility, but it could make a difference if we were nudged in the right direction.
When it comes to the public wallet, hypertension accounts for billions of dollars in healthcare costs, according to Dr. Campbell. ‘And since it’s almost completely preventable, that’s arguably not an acceptable situation,’ he says.
6. How many readings should you have?
It’s recommended that doctors have patients sit calmly for the first reading and then take a couple more, one to two minutes apart, before averaging those measurements. If hypertension is in the mild to moderate range, a follow-up appointment should be made to take readings again.
‘There’s a lot of overdiagnosis and subsequent overtreatment of hypertension,’ says Dr. Leenen. ‘If you’re borderline, then you should come back in two or three months to monitor it.’ When readings are repeatedly above 140/90 in the doctor’s office and 135/85 at home, then the patient is usually considered to have hypertension.
About 20 percent of us register abnormally high readings when our blood pressure is taken at the doctor’s office but normal readings at home. This phenomenon, called ‘white-coat hypertension,’ probably results from feeling a bit nervous in a hospital or clinical setting. On the other hand, about eight percent or more have readings that are below the hypertensive threshold at the doctor’s office but are actually hypertensive at home. This is known as ‘masked hypertension’ and may go undetected for years.
7. What else should be done if your readings are high?
Any hypertension results should trigger a careful analysis of medical and family history, as well as tests to investigate other risk factors, such as blood or urine analysis for cardiovascular disease, diabetes, kidney damage, gout and arthritis. The higher your risk factors for cardiovascular disease, the more important it is to lower your blood pressure.
8. Which lifestyle changes make a difference?
Five key behaviours can have a big impact on blood pressure: exercising four or five times a week, reducing alcohol consumption to less than three drinks a day for men and two for women, reducing salt consumption (particularly in processed foods), maintaining a healthy weight and increasing fruit and vegetable intake. Quitting smoking and managing stress are also good moves, and recent studies suggest that reducing sugar intake, even without weight loss, is another step that can improve blood pressure.
These lifestyle factors have the added benefit of being ‘the same ones that help prevent obesity, diabetes, cancer and all the greatest threats to our lives,’ says Dr. Campbell. ‘Ideally, everyone should implement them, whatever their blood pressure.’
9. How difficult is it to make lifestyle changes?
Developing heart-healthy habits can be challenging. Even so, there are examples of Canadians who have managed to turn their daily routines around. When Ryan de Gans was diagnosed with hypertension at the tender age of 21, he took it as a cue to ‘figure himself out.’ The Edmonton native was under a lot of personal stress, and his anxiety caused repeated panic attacks. He also had a habit of drinking heavily with his buddies. After his doctor told him that he had high blood pressure ‘ even when he was in a calm state ‘ he quit smoking and alcohol, took up regular exercise and found rewarding new work as a business development consultant.
‘A lot of physical changes came out of my new way of life, but the real change took place in my mind,’ he says. ‘I found a vision for my future. I found value in my life. I found a reason to want to be fit and healthy.’
Failure to make a major lifestyle change may lead to indefinite pharmaceutical treatment. This, in itself, can be difficult, says Rhian Touyz, a leading hypertension expert from Scotland. ‘Patients become apathetic about taking medication daily for life,’ she says. ‘That’s why it’s so important to have regular contact with your doctor and regular motivation from healthcare providers.’
The consequences of uncontrolled hypertension can be dire. According to the Heart and Stroke Foundation, it’s a leading risk factor for heart disease and stroke, two of the three most common causes of death in Canada that are responsible for more than 69,500 and 14,000 deaths annually, respectively.
10. If I take medication, will there be side effects?
Many types of medication are now available. Everyone should be able to find a drug or combination of drugs that controls blood pressure with minimal to no side effects.
Some hypertension medications may cause diarrhea or other gastrointestinal problems. For example, olmesartan ‘ an angiotensin receptor blocker (ARB) with the trade names Benicar, Azor and Tribenzor ‘ has been associated with celiac-like changes to the intestine. Tell your doctor about any side effects.
Sometimes the process is one of trial and error. Fifty-six-year-old Montrealer Ray Taylor started off with a low-dose ARB, but his blood pressure was still high after a month. His doctor doubled the dose, then added a diuretic to the mix before Taylor’s reading finally reached the target range. ‘Altogether, it took about three months to get to a place where it was working,’ says Taylor. But he had no side effects and started feeling better almost right away.
‘At first, I was a bit nervous about how it would go, just like anybody starting a new medication,’ says Taylor. ‘I don’t like to think of myself as a guy who takes pills, but the consequences of heart disease are a lot worse. My message to anyone in the same boat is ‘Don’t put it off.”
Related:
‘ Why Hypertension is a Silent Killer
‘ 5 Ways to Reduce Your Risk of High Blood Pressure
‘ Eat Your Way to Lower Blood Pressure




