Psoriasis
If you thought you’d never wear shorts again because of your blotchy, flaking skin, take heart. You will be glad to hear that treatment options for unsightly psoriasis have doubled in recent years.
Source: Adapted from Knowing Your Options: The Definitive Guide to Choosing The Medical Treatments, Reader’s
What is psoriasis?
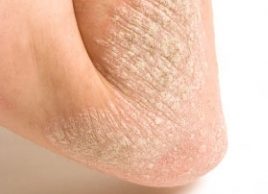
This chronic skin disease isn’t easy to ignore: Its raised red patches covered with silvery scales itch (fittingly, "psoriasis" comes from the Greek for ‘itch’). Your self-image may suffer if it spreads. Psoriasis occurs when production of new skin cells outpaces the rate at which old ones are shed. As a result, live cells accumulate in raised areas covered with whitish flakes of immature skin cells (or plaques). Researchers say this rapid cell turnover relates to an inherited immune system disorder that can be activated by stress, cold weather, infection, or an abrasion.
Plaque psoriasis often appears on elbows, knees, palms, soles, the lower back, and the scalp. Less common forms of psoriasis include: guttate, with teardrop-shaped spots; pustular, with pus-filled skin lesions; inverse, appearing in skin folds; and erythrodermic, with widespread skin scaling and inflammation. Psoriasis flares up periodically and can persist for long periods before going into remission. Although it occasionally covers large areas, this condition is usually mild and manageable. Nearly one-third of patients develop psoriatic arthritis.
Treatment for psoriasis
There is no cure for psoriasis, but you can control it and minimize its symptoms. Milder cases of psoriasis usually respond well to OTC and prescription topical drugs and shampoos, in addition to sunlight. For more severe cases, you’ll need oral drugs and specialized light therapy. Most doctors use a combination of treatments, and you may need to experiment to find the mix that best suits you.
Medications for psoriasis
Most psoriasis requires medication. To begin, a topical formulation (cream, gel, ointment) can help. Try OTC salicylic acid (Hydrisalac) to dissolve scales, or coal tar gels to slow skin cell growth. Prescription topical corticosteroids can reduce more severe inflammation. (An occlusive tape, called Cordran Tape, has corticosteroids in it.) Daily use of a topical corticosteroid such as halobetasol (Ultravate), is a common regimen for more severe psoriasis. After the patch clears up, apply just on weekends. You can also combine weekend steroid use with weekday use of calcipotriene (Dovonex), a form of vitamin D3.
For scalp psoriasis, try a medicated shampoo such as coal tar (Denorex Medicated) or anthralin (Dritho-Scalp). Both stain, and anthralin can irritate normal skin, so use them carefully. Tazarotene (Tazorac) or salicylic acid shampoo (DHS Sal) may slow flakes, too. There’s also a fast-acting but expensive steroid foam.
For severe psoriasis, an oral immunosuppressant drug such as cyclosporine (Neoral) or methotrexate (Rheumatrex) may be needed. Once it begins working, an oral retinoid (vitamin A derivative), usually acitretin (Soriatane), is added. The immunosuppressant is then gradually withdrawn and a low-maintenance dose of Soriatane continued. Doctors also recommend rotational therapy’switching approaches after a couple of years’to prevent serious side effects or resistance to a drug’s benefits. Immunotherapy agents have been approved for treatment of moderate to severe psoriasis.
Lifestyle changes
The first relief for your psoriasis is as close as your yard or rooftop: Expose affected areas to sunlight, but not sunburn, for 15 to 30 minutes a day. This brings improvement within six weeks in about 80% of people who try it. (Be sure to protect unaffected areas with sunblock.) Soaking in a bath solution enhanced with coal tar, Dead Sea or Epsom salts, or colloidal oatmeal (Aveeno) can soften scaly psoriasis buildup. As soon as you get out of the tub, apply a heavy moisturizer, such as Cetaphil, Eucerin, or petroleum jelly, to soften and soothe your skin. Your doctor may also recommend watertight (occlusive) tapes, especially if you have psoriasis-related cracks on your palms and soles.
Related procedures for psoriasis
With moderate to severe psoriasis, you’ll need light therapy with ultraviolet B (UVB) rays at your dermatologist’s office, a hospital, or with a home unit. For more severe psoriasis, a special therapy called PUVA combines the oral drug psoralen with deeper-penetrating ultraviolet A (UVA) rays. Such treatments are very effective but can up your skin-cancer risk.
Questions for your doctor
‘ When can I expect to see some improvement?
‘ How far is my psoriasis likely to spread?
‘ I’m trying to conceive. Which psoriasis drugs are unsafe for me?
Living with psoriasis
If you’re living with psoriasis, here are a few quick tips to help you take control:
Be aware certain drugs can make your psoriasis worse. Lithium, antimalarials, and such heart drugs as ACE inhibitors and beta-blockers are the worst offenders.
Winterize your program. Winter’s dry, cold air can mean more psoriasis. Be careful not to scratch; it can make lesions worse. Instead, slather on moisturizer more thickly, applying it while your skin is damp, and get some sun (using sunblock, of course). What better excuse for that tropical vacation?
Try meditation or relaxation techniques if your psoriasis flares up under stress. They can help you deal with life’s pressures.




