My Cousin Gave Me Her Kidney—And Saved My Life

With my kidneys failing and an interminable waiting list for an organ donation, my situation was dire—until I received the ultimate gift.
The subject heading on the email was surprisingly mundane: “Final pre-op appointment letter.” It sat in my inbox for hours before I finally opened it, believing it was just another pre-screening for the kidney transplant I desperately needed. There was a list of appointments and test dates, and at the bottom—almost as an afterthought—it said: “Your kidney transplant surgery has been scheduled for Thursday, June 13, 2019.”
I stopped cold. I had to reread that line several times before I could start to grasp what it really meant: my cousin Christine really was going to risk her life in order to save mine.
Back in January 2018, at age 37, I had started feeling exhausted and extremely itchy and cold all the time. I chalked it up to dry, winter skin and working too hard. Another two months passed before I tested my blood pressure at the grocery store, and the shockingly high reading prompted me to make a doctor’s appointment.
My GP ran a few tests, and I continued on with my life. I’m a television reporter at CityNews Toronto, and I was in a car heading to an interview when I got the call: my kidneys were failing. On my doctor’s advice, I hightailed it to the nearest emergency room, and was admitted.
There I was, decked out in a hospital gown with camera-ready hair and makeup. I couldn’t believe what was happening—even though kidney disease runs in my family. My father had spent four years on dialysis before receiving a transplant; he passed away at 50 from a complication of the disease. I knew that I had inherited a rare kidney condition, Alport syndrome, from my dad, but I had been regularly monitored until I was 18, and my doctors didn’t think it would be an issue. Most women who have it are carriers but don’t have symptoms. I was supposed to be in the clear.
My mother immediately started the process for becoming a living donor. But she had to lose 50 pounds before her application would be considered. While she got on the treadmill, my kidney specialist and his team tried to help me stave off complete organ failure. He was frank about my situation, but optimistic. He told me I would need dialysis and that with end-stage kidney failure I was essentially sterile and unlikely to be able to have children until I received a transplant. And if I didn’t get a transplant, I would eventually die.
Many doctors would have rolled me straight to surgery to install the dialysis equipment, but he thought I might be able to avoid it with the right combination of vitamins, prescription drugs and dietary changes—and if I didn’t have to wait too long for a transplant.
After three days, I was released from the hospital but returned for countless blood tests and appointments. I also had to go through a transplant workup: ultrasounds, cardiovascular tests and even vascular tests to see if I was able to undergo hemodialysis (having blood removed and cleaned through a machine, then pumped back in).
My diet changed dramatically, too; no more Diet Cokes, no more pickles and no more cheese, because my body couldn’t filter out all the phosphorus and sodium. I had to limit my liquid intake to less than 1.5 litres a day and chewed gum to quench my thirst. I had to take a battery of pills—vitamins, minerals and prescription drugs—and get weekly shots to keep my hemoglobin levels high.
After five months, my kidney function dropped further, and my symptoms got worse. I had restless-leg syndrome and could barely sleep; I was so exhausted that some days I couldn’t get out of bed. Seemingly easy tasks, like putting away laundry, became monumental. Though the process to determine if my mother could be a donor was still under way, I couldn’t wait much longer. In August 2018, a catheter was inserted into my stomach. By September, I was doing peritoneal dialysis every night at home in order to do the work my kidneys usually do. For nine to 10 hours at a time, I became a prisoner to my dialysis machine.
During this time, my mother lost the weight, but due to the reduced kidney function that comes with age, she was ultimately deemed an unsuitable candidate. I was put on the wait-list for a deceased donor, but I was advised that, given my blood type, I wasn’t likely to be called for seven years—if I could survive that long.
And then Christine stepped up.
(Related: How Trey Anthony Found Strength Through Vulnerability)
My extended family is fairly close, but I didn’t spend much time with my cousin Christine Hodgkinson when we were kids. She’s 17 years older than me, so she wasn’t a playmate; she was someone I looked up to. I remember being eight or nine and asking her if I would get her high cheekbones and beautiful eyes when I grew up. Little did I know that I would end up getting something else instead.
Christine, a mother of five in her mid-50s, had already gone through the process to be a living donor when her father-in-law needed a transplant several years before. She was a match, but a blood relative was ultimately a better option. Now here she was willing to go through it all again.
Familial organ donations are often best, and recipients of organs from a live donor typically have better outcomes. Transplant coordinators will only look at one candidate at a time, so once my mother was off the list, my sister—who isn’t eligible to donate because she shares the same genetic variant as me—immediately called Christine, who had offered to be tested when I was first diagnosed.
I didn’t want to put Christine in a difficult position by reaching out to her directly. It’s not exactly an easy ask. You aren’t borrowing a dress or even a couple thousand dollars—you are asking somebody to undergo major surgery. The procedure for a living donor can be longer and riskier than that of the recipient. Kidneys are protected by a variety of other organs, which means there’s a chance that those organs and their surrounding tissue could be injured during the removal process. Even if the transplant was a success, she would still assume the potential for future high blood pressure or kidney problems, among other issues—all so I wouldn’t have to be tied up to a dialysis machine every night.
Despite the sacrifices, Christine told my sister she would do it. After she completed the initial tests, it took five months to confirm that she was a suitable match. Although she was busy helping to care for her seriously ill father, Christine regularly made the 90-minute drive from her Keswick, Ont., home to downtown Toronto for testing. Sometimes the tests were scheduled so early that she’d leave home before dawn or stay in a hotel the night before.
Christine and I had our final pre-op appointments on the same day, and that’s when the reality of what we were doing sunk in. I was petrified about what could happen to Christine and to me. What if the transplant didn’t work?
Two days later, I called Christine to see if she would be okay with postponing the surgery for a few weeks. I felt like I needed more time to process what was happening. She talked me off the ledge, reassuring me that she knew the risks and was willing to take them. Then we joked about how horrible our hair would look after spending days in the hospital. By the end of our call, I felt reassured that Christine truly wanted to do this—and so did I.
Christine and I didn’t get to see each other on the morning of the transplant. She went into surgery hours before me, while I was surrounded by family in the waiting area. Surgeons removed her kidney, staff cleaned the operating room and then the team transplanted her kidney into my body—close to my groin, attached to the femoral artery, leaving my non-functioning kidneys in place because removing them could harm my other organs.
Hours after the surgery, I woke up to cheers from the street: the Toronto Raptors had just won their first NBA championship. Those hoots and hollers weren’t for Christine or me, but they may as well have been. For the first night in 10 months, I wasn’t plugged into a dialysis machine.
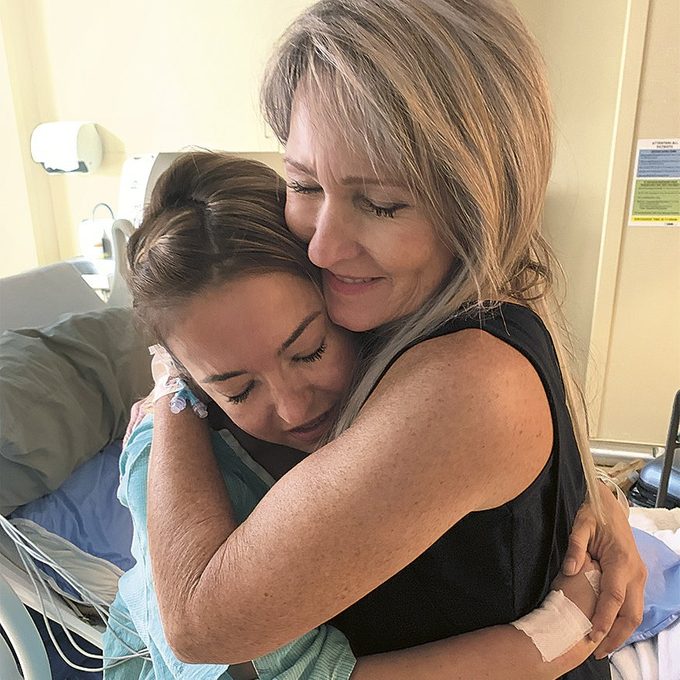
I spent the next few days in a drug-induced haze in the equivalent of a transplant-only ICU, while Christine recovered on another floor. When we finally saw each other in my room, the newly formed bond between us was remarkable. I felt completely linked to her, like we were sisters. She would never again be a cousin who I only saw at holidays and weddings. I had a girlfriend visiting at the time, and Christine put her phone in camera mode, handed it over to my friend and then gave me a giant hug. That photo, which is displayed in my home office, is now an iconic one in our family.
Christine was discharged a few days later and spent the summer recovering with seemingly no setbacks. My recovery was more gradual, but I felt the impact of her kidney almost immediately. After I sobered up from the pain meds, I felt years younger. I didn’t have to drag myself out of bed or deal with hours of dialysis every night—and I could last an entire day without needing a nap.
(Related: 17 Gratitude Quotes That Can Help You Feel Grateful)
Although I’m on the other side of my surgery now, I will always have kidney disease. I need to take certain medications for the rest of my life; the immunosuppressants I’m on—to ensure my body doesn’t reject the new kidney—make me vulnerable to disease and viral infection. They also have radically increased my risk of skin cancer, so I can’t go outside without lathering up in sunblock. I go for blood work every week, and if my levels of creatinine (a toxic waste product) are too high, I’ll be readmitted to hospital.
That’s what happened on Labour Day weekend in 2019. I was ready to go away with my partner on our first overnight trip in years where we didn’t have to bring a 50-pound dialysis machine and enough supplies to be mistaken for exhibitors at a medical trade show. We were about to leave the house when I got the call.
My creatinine levels were rising: they were more than double those of a healthy person, and my nephrologist wanted to admit me to the hospital. He was concerned that my body was rejecting Christine’s kidney. When I got off the phone, I sat on the floor of my bedroom, next to my suitcase, and sobbed—about the potential loss of the kidney, what that would mean for my gradual return to normalcy and also the horrible possibility that all of Christine’s heroic efforts might have been in vain.
I told just a handful of people that I was back in the hospital; I decided only to let Christine know if things escalated. My doctors weren’t sure what caused the spike, but after two days on an IV, my creatinine levels started returning to normal.
I was waiting to be discharged when Christine sent me a text. “Hey there. How are you feeling? Hope everything is still going well.” We hadn’t spoken in about a week. I told her about the false alarm. She’d later tell me that she felt something was wrong all weekend.
A few weeks after my scare, Christine told me that her single kidney had grown (which is common for solo kidneys as they pick up a bigger workload) and she now had 70 per cent functionality. That was the first night in months where I slept soundly. We were both going to be all right.
I returned to work in October 2019 and feel even more invigorated than before my diagnosis. I’m able to fully enjoy life, whether it’s going to my annual girls’ Christmas party without falling asleep on the couch or taking long walks with my partner.
A year ago, I was tied to a machine every night, dreaming of better days. Now they’re here.
© 2020, Cristina Howorun. From “My Cousin Gave Me Her Kidney and Saved My Life,” Chatelaine (January 9, 2020), chatelaine.com.




